It has long been established that junk food advertising drives consumption of unhealthy food and drink, shaping preferences from a young age and contributing to overweight and obesity.
The strength of the evidence base is perhaps best corroborated by the enormous advertising budgets of unhealthy food and drink companies. If advertising didn’t pay off, why would Coca-Cola allocate a whopping $5 billion to their worldwide advertising budget in 2024?
Restricting junk food advertising is therefore a powerful and proven public health measure. Yet, most recently, you may have seen measured responses from public health advocates in the UK, including World Cancer Research Fund, upon the introduction of long-awaited junk food advertising restrictions in January 2026.
Marketing regulations can underdeliver
The bottom line is that whilst the UK’s restrictions mark a step forward in protecting children’s health at a time when obesity rates continue to rise, they have been weakened and delayed by industry influence – most notably through the introduction of a sweeping brand exemption. This significantly undermines the policy in two key ways. First, it allows brands that are synonymous with foods high in fat, salt and sugar (HFSS) to continue being advertised – think the famous Golden Arches. Second, the lack of brand restrictions enables companies to promote entire HFSS product ranges, just not individual products. Ultimately this preserves brand visibility and influence while circumventing the spirit of the regulations.
The brand exemption is not the only weakness of the advertising restrictions. Work on this policy began as far back as 2018, and in the years since, the marketing landscape has evolved dramatically. Simply put, the regulations are not a match for the rapidly changing marketing landscape. For example, direct marketing channels, such as email and text messaging, remain unchecked, allowing unhealthy food and drink companies to continue targeting consumers.
The unseen cost of delays and dilution
The unfortunate tale of industry influence is not unique to the UK. Globally, efforts to curb the scourge of junk food on society are denied, diluted, derailed and delayed by industry.
Marketing restrictions are difficult to get over the line. In the UK, the policy was subject to five separate consultations and four delays to its rollout. That is an immense amount of government time, effort and resources. Moreover, the burden it places on the public health sector, which often operate under capacity constraints, must be acknowledged.
We also need to recognise that obesity, a key risk factor for cancer, is linked to deprivation. In many countries, those living in the most deprived areas are more likely to be living with obesity compared to those in the most affluent communities. Delays or failures to implement effective policies therefore disproportionately impact those who are already most vulnerable.
Industry opposition at full throttle
The resistance we see to advertising restrictions can partly be explained by the fact that marketing is not a peripheral commercial function. Instead, it sits at the very core of food and drink businesses, playing a pivotal role in building brand value, customer loyalty and long-term profitability.
Marketing restrictions are also unusually visible. Unlike reformulation targets or nutrient thresholds, which operate largely behind the scenes, advertising bans are immediately noticeable. They can also be drawn into wider debates around personal responsibility, censorship and creativity – making the more contested and politically charged. They tend to hit a nerve.
Recognition of these issues is not a justification for inaction. The reality is that companies by their very nature are required to innovate, and they can do so in a way that supports public health rather than undermining it.
Action must go beyond the status quo
Let’s be clear, no one is suggesting that junk food marketing restrictions alone will solve the obesity crisis. However, the version we’ve seen introduced in the UK will most certainly underdeliver, especially given the restrictions don’t sit within a broader framework of measures designed to improve the nation’s diet yet. Countries in Latin America, including Chile and Mexico, have taken more holistic approaches which embed marketing restrictions within a wider set of measures including mandatory warning labels and robust school food standards
But when governments introduce policies that appear ambitious on paper but lack the strength to deliver in practice, they risk entrenching the status quo while giving the impression of action. This pattern is not unique to food. Similar delays and dilutions are seen across alcohol, gambling and other health-harming industries, where commercial interests routinely take priority over public health.
Ultimately, the question is not what needs to be done, but what governments are willing to do to protect public health.
Today the UK Government published a long-awaited update to the Nutrient Profile Model (NPM) – a quiet but powerful public health tool that is central to cancer prevention and tackling diet-related diseases.
NPMs are used to assess how healthy foods are, classifying products as healthier or less healthy (often referred to as HFSS – high in fat, salt and sugar). While no system is perfect, the NPM is critical because it underpins food policy, determining which products are captured by regulation and which are allowed to escape it.
The UK’s existing junk food advertising and promotion restrictions are still based on the 2004 NPM. This means the effectiveness of these policies depends entirely on a model developed more than 20 years ago.
A robust, evidence-based NPM is essential to prevent unhealthy products continuing to fall through regulatory gaps. Since the original model was developed, the science on diet and health has moved on.
Obesity firmly established as major driver of cancer
In particular, evidence linking unhealthy diets, overweight and obesity, and cancer risk has grown substantially. Obesity is now firmly established as a major driver of cancer and one of the leading preventable causes of the disease in the UK and globally. If food policy is to meaningfully improve diets and reduce obesity-related cancer risk, it must be built on a credible, up-to-date NPM.
Importantly, the updated NPM will better reflect recommendations from the independent Scientific Advisory Committee on Nutrition (SACN) on free sugars and fibre, ensuring policy aligns with current scientific guidance.
We therefore warmly welcome today’s publication of the revised NPM, first consulted on in 2018. This is an important step forward. However, the updated NPM is not yet applied in policy.
The Government has committed to holding a public consultation in 2026 on applying the 2018 NPM to advertising and promotion restrictions. We stand ready to work with the UK Government at this next stage to ensure the NPM delivers real progress for cancer prevention and overall public health.
There aren’t many things in life you run straight into without testing first. Plays need rehearsals, restaurants need test kitchens, and researchers need feasibility studies.
Think about pilot and feasibility studies like the first walk-through of a play. You’re planning a large-scale production, and you want it to be a success – you can’t just go straight into the performance. First, you need to suss out: have you got the script right? Can you get the actors in the roles? Will the show be a hit?
It’s the same with feasibility studies. Before you run a big trial, with a lot of time, funding, and resources thrown into it, you need to figure out whether the whole thing is actually possible!
What do pilot and feasibility studies aim to achieve?
The aim of both pilot and feasibility studies, yes – you’ve guessed it – is to see if a study is feasible. A pilot study tests the exact design of a larger future trial; it’s essentially a mini version. A feasibility study differs in that it doesn’t have to follow the exact design of the planned trial, instead it can explore various aspects of the study’s design to find out what works best.
These studies are the prime time to ask key questions and put them to the test in real life. These include questions about:
- Recruitment and retention: can you realistically get enough people to take part in the trial? And not only will they sign up, but will they stay for the whole duration?
- Acceptability and adherence: are participants and staff happy with the study plan and assessments that are carried out? And do they follow it as planned?
- Data: is the data collected reliable, complete, and good quality?
- Resources: have you factored in all the relevant ingredients? Do you have enough time, staff and money to run it as planned?
- Method: is this study recipe one that can be followed smoothly?
- Safety: are there any safety concerns that could prevent scaling up?
Without testing, it can be hard to know. The science could be spot on, the study beautifully designed, but if participants don’t like it or professionals find delivering it a burden, then you don’t have a successful trial on your hands.
Therefore, researchers take this chance to identify and explore potential challenges before the main trial begins. By tackling these issues early, you’re less likely to face unexpected problems or setbacks further down the line.
Feasibility studies also represent the first touch point with real people that could be involved in the research. This allows the target group to be the central focus and understand what works for them. This opens up the opportunity for researchers, clinicians, and participants to collaborate and learn how best to conduct the study.
Funding pilot and feasibility studies
Once you’ve got the findings from your feasibility trial, it’s going to be much easier to progress to running the actual trial, because you’ve rehearsed it. Not only that, but it will also help secure the funding needed to run the bigger trial. After all, they’re not cheap. Being able to show pilot or feasibility data to funders proves that you’re coming to them with a tried and tested plan, boosting the chances that the main trial will be achievable.
That’s why at World Cancer Research Fund International, we offer specific grants for pilot and feasibility studies, as part of our Regular Grant Programme. These are for shorter time periods, with lower budgets than our investigator initiated grants.
Sometimes they prove to work well and achieve the intended results.

Dr Campbell
One example is our grant holder Dr John Campbell, who ran a pilot trial to assess whether a 16-week exercise programme for people with chronic lymphocytic leukaemia (a type of rare cancer of the blood and bone marrow) was safe and acceptable.
The study concluded that the programme was both safe and feasible, and even showed an increase in muscle mass and reductions in fat around the lower body.
Dr Campbell and his team also received positive feedback from the participants in the study, with one saying:
“I have strong memories of the trial. It came into my life during some dark days and gave me a sense of routine and a newfound purpose. I’m so grateful for the opportunity to meet the researchers, though I wish it had been under different circumstances.”
Dr Campbell and his team now plan to use this small-scale study to inform a larger trial that will, for the first time, assess the tumour-suppressing effects and mechanisms of exercise in chronic lymphocytic leukaemia.
Sometimes pilot studies can highlight challenges and important considerations for a study’s design. And these results are just as important.
Not only does this save a lot of time and money on a trial that won’t succeed, but it’s also an essential way to learn what doesn’t work, so other researchers can avoid encountering the same issues.

Prof Craike
Take, for example, a project led by grant-holder Prof Melinda Craike and funded by our network charity Wereld Kanker Onderzoek Funds. The study examined the feasibility of a nurse-delivered physical activity promotion intervention for prostate cancer survivors living in socio-economically disadvantaged areas. Recruitment was low, and both nurses and survivors reported only low to moderate acceptability. Survivors highlighted barriers such as a lack of interest, perceived cost, other health concerns, and a preference for advice from their general practitioners.
Rather than going ahead with a costly full-scale trial, Prof Craike and her team concluded the intervention was not feasible in its current form. Importantly, they also offered guidance for future research, such as exploring incentives for participation, involving GPs in delivery, and using community-based participatory approaches.
Prof Craike explains:
Pilot and feasibility studies might not always produce the results researchers expect, but they always offer valuable insights. I encourage the publication of feasibility studies, including those that are unsuccessful, to reduce waste and duplication, and to inform the development of future research efforts. Even though they are often unpublished, reporting unsuccessful feasibility studies like ours is essential to protecting research resources and guiding future projects.
Far from being ‘failures’, pilot and feasibility studies are crucial for developing smarter, more sustainable research.
The UK Women’s Cohort Study (UKWCS), which we provided initial funding for, recently celebrated its 30th anniversary! This is an incredible achievement because many research projects only last a couple of years. Such a long-term project can provide scientists with richer, more detailed information to help prevent cancer.
The UKWCS, led by Prof Janet Cade from the School of Food Science and Nutrition at the University of Leeds, is one of the largest cohort studies investigating diet and cancer in the UK, comprising over 35,000 middle-aged women and representing a wide range of different eating patterns, which can help scientists research what protects against cancer and coronary heart disease. Participants are regularly followed up to examine what effect food and nutrient intakes have on their long-term health.
Preventing cancer through what we eat
The first survey was funded by World Cancer Research Fund and the data produced from this survey and later ones has been used to investigate:
- meat and fibre intake and breast cancer
- vitamin C supplementation and breast cancer
- fibre intake in type 2 diabetes and cardiovascular disease
Over 3 decades, these investigations have provided interesting findings. For example, women who eat more fibre have a lower risk of stroke, and women who eat more red and processed meat have a greater risk of developing breast cancer.
Of course, we do not eat specific nutrients alone, so dietary patterns have also been identified and explored. Compared with meat eaters, vegetarians and fish-eaters (non meat-eaters who do eat fish) may have some protection against post-menopausal breast cancer.
This wide-ranging set of data can be used to identify common trends and to help target health information. For instance, women who eat more fruit and vegetables tend to be vegetarian or vegan, to take vitamin or mineral supplements, to be married, to be non-smokers, and to be educated to at least A-level or degree level.
To celebrate the milestone, World Cancer Research Fund hosted a party for colleagues who have worked with UKWCS over the last 30 years, in person and online from all over the country. Prof Cade talked about the UKWCS, and gave us some reminders of how different the world was 30 years ago. Diet is complex, so we need to understand how various factors interact to influence our health. It was fantastic to hear about all the findings so far from the project, and see so many people in the room who could share memories of working together.
Dr Darren Greenwood shared some reflections about the history of the UKWCS and its origins, from when we awarded the University of Leeds funding to investigate links between diet and cancers. The UKWCS grew and grew as more researchers worked with the data, and were awarded further funding. Sadly some members of the original cohort have died since the study launched. Yet Dr Greenwood reminded us that this data tells a story that helps us decode how to prevent cancer, and help people live longer, healthier lives.
This legacy is one of the enduring strengths of the UKWCS. The study has been cited in at least 9 government policy documents, providing direct life-changing information to help improve health and lives on a population scale.
Dr Diane Threapleton is one of the researchers who has used UKWCS data, including looking at how increasing fruit and vegetable intake slows weight gain. She focussed on the women of the study, highlighting how the data, time and samples they provided open a vital window into how what we eat interacts with real life. This was a timely reminder of the contributions of the women of the study, without whom none of this would have been possible.
Insights into ageing and beyond
After this, we heard from Yuanyuan Dong, who is working with the UKWCS to examine how diet affects the risk of rheumatoid arthritis. Yuanyuan joined us online from China, highlighting the global reach of the experts working with the cohort.
Finally, Dr Sarah Jing Guo told us about her plans for the UKWCS data – looking to the next 30 years! She gave us details of what her PhD student, Xinyue Liu, is examining with her project looking into how replacing processed meat with unprocessed meat or dairy products affects the risk of developing type 2 diabetes. She also gave us insights into how the cohort data could aid research into an ageing population, looking at Parkinson’s disease, Alzheimer’s or musculoskeletal disorders.
This amazing piece of long-term research is an important reminder of how small seeds of funding can have an impact over many decades and even lifetimes. We’re truly grateful to the donors of 30 years ago who helped make this research happen.
> More details about the UK Women’s Cohort Study, including information about publications

Documents from the UK Women’s Cohort Study

Help us fund the research of the future
Gifts in Wills help us fund long-term research projects like Prof Cade’s
 We spoke to Dr Renate Winkels (pictured) and Dr Laura Winkens, at Wageningen University & Research, to discover more about their studies in bowel (also known as colorectal) cancer.
We spoke to Dr Renate Winkels (pictured) and Dr Laura Winkens, at Wageningen University & Research, to discover more about their studies in bowel (also known as colorectal) cancer.
Your team looked at what influences people’s health behaviours after they’ve been treated for bowel cancer. What do you mean by health behaviours and what did you find out?
Health behaviours are the everyday choices people make that affect their health. In this study, we focused on 2 things:
- healthy eating (more fruit, vegetables, whole grains and beans; and less fast food, red meat, processed meat, sugary drinks and alcohol)
- physical activity
For people who’ve had bowel cancer, healthy behaviour may be associated with living longer, feeling better and having fewer problems like fatigue.
However, in previous studies, we found that many bowel cancer survivors don’t make big changes after treatment. Survivors are dealing with side-effects from the cancer or its treatment (such as gastrointestinal problems, fatigue or body image distress), which can make it hard to eat well and stay active.
Our study looked at what helps or gets in the way of healthy behaviour for people who have finished treatment for bowel cancer. We found:
Personal factors matter
How much time people have, their motivation, what they believe about healthy habits, what they know, and the skills they have can all influence whether they eat well and stay active.
Support helps
Encouragement and support from family and friends, or feeling like healthy habits are normal in their social circle, can make a big difference.
Environment plays a role
Access to gyms, parks, or even just good weather can affect how easy it is to be active.
Cancer symptoms can get in the way
Ongoing physical issues after cancer treatment, like fatigue or bowel problems, often make it harder for people to stick to healthy habits. But if someone is feeling physically well, they’re more likely to eat better and stay active.
Mental health may be important
Depression or being unhappy with one’s body seem to be linked with less healthy behaviour.
In short, to help people with bowel cancer lead healthier lives after treatment, we need to focus on motivation, knowledge, support, and overcoming the challenges they face physically and emotionally.
Towards a more complete picture
Your team conducted a “systematic review”. What is that and why is it important?
We wanted to find out what other scientists had studied, so we could build our study on the latest evidence. Moreover, we wanted to provide an overview of the topic. We looked at 21 papers, but we started with around 800 publications, and had to sift through them to identify the relevant ones.
You divided the studies into quantitative or qualitative. Why did you choose to look at both?
Quantitative studies collected a lot of numbers and measurements. The studies used standardised questionnaires to collect data on dietary intake and other aspects of lifestyle. Those studies answer questions like “how many” or “how much”.
Qualitative studies focus more on experiences. Such studies are mostly interviews to better understand why people do what they do, or how people behave.
Together, they provide a richer, more complete picture of the challenges and motivations colorectal cancer survivors face.
Were you surprised that people find it hard to change their behaviour?
Not really. Most people will recognise how challenging it can be to always make healthy choices. After cancer, when you’re rebuilding your life, that can be even harder.
How important is mental health for people living with and beyond bowel cancer?
Mental health is a very broad topic. People who have had bowel cancer may have a stoma, or be suffering from fatigue, or from bowel functioning problems. These can have a real impact on your life, and it’s important to address them. Some care teams really have an eye on this, but it’s not always the case. One patient told me that she did not dare to discuss her feelings of severe fatigue with her oncologist, as the oncologist told her that “fatigue was not a thing” for people with bowel cancer. We need more awareness and integrated care that addresses both mental and physical health to truly support survivors’ wellbeing.
You’ve also looked at whether following our Cancer Prevention Recommendations can reduce fatigue for people with bowel cancer.
We set up a study to assess whether following the Recommendations would help people to feel less fatigue. Cancer-related fatigue is a symptom that many bowel cancer patients experience during treatment and after completion. What is disturbing is that this type of persistent, overwhelming sense of physical, emotional or mental fatigue is not proportional to activity nor relieved by resting or sleeping.
We recruited participants for the trial who were experiencing cancer-related fatigue. In a randomised study, half of the group received lifestyle coaching to improve their adherence to the Recommendations, while the control group did not.
The coaching really helped the participants to adopt a healthier lifestyle: over time, this group reported eating more fruit and vegetables, and less processed meat and sugar-sweetened beverages. Also, physical activity levels went up more in the group that received coaching than in the control group.
Nevertheless, those changes didn’t result in less fatigue. This suggests that while these changes have many benefits, managing fatigue may require additional, targeted interventions.
This grant was funded by Wereld Kanker Onderzoek Fonds based in the Netherlands, as part of the World Cancer Research Fund International network.
Key takeaways:
- The CO21 CHALLENGE Trial found that a structured exercise programme after chemotherapy led to a 28% lower risk of cancer recurrence in colon cancer survivors compared with usual care.
- This is the first randomised controlled trial (RCT) to show that exercise directly improves survival in colon cancer patients. It confirms what observational studies have long suggested.
- The results were presented at a recent conference and made headline news. Experts say the CHALLENGE Trial marks a shift from viewing exercise as a “nice to have” to a “need to have” in cancer care.
Colon (part of the large bowel) cancer survivors who took part in a 3-year structured exercise programme had a 28% lower risk of cancer recurrence or a 2nd cancer. They also had a 37% lower risk of death compared with usual care.
These findings were shared at the 2025 Association of Clinical Oncology (ASCO) Annual Meeting. They were also published in the New England Journal of Medicine.
The ASCO Annual Meeting is the world’s largest oncology conference. It attracts more than 40,000 attendees from around the world. Every year, ASCO highlights the latest advancement in treatments. It also shares the directions that have the greatest potential for progress and patient impact.
Spotlight on exercise
The CO21 CHALLENGE Trial pulled back the curtain on a weapon that has been hiding in plain sight: physical activity. The results of the trial showed improvement in disease-free survival and overall survival in colon cancer survivors in the aerobic exercise intervention group. This trial is the first gold standard RCT to show what has long been indicated from observational studies. This is a big deal!
The impact of exercise on cancer outcomes has been a topic of great debate. Observational research has shown improvements in survival and quality of life linked to higher levels of physical activity. However, observational study designs are limited. They do not show cause and effect.
Plus, they are hard to implement in clinical settings due to concerns that the reported effects may not truly reflect the impact of exercise (and may be due to something else).
Our research
Over the past few years, World Cancer Research Fund International has done extensive reviews through its flagship Global Cancer Update Programme (CUP Global).
CUP Global includes partnerships with American Institute for Cancer Research, World Cancer Research Fund in the UK and Wereld Kanker Onderzoek Fonds in the Netherlands.
Our CUP Global reviews look at the extent to which diet, nutrition and physical activity impact people after a diagnosis of breast and colorectal cancers with regard to:
- cancer-specific mortality
- all-cause mortality
- risk of cancer recurrence
- health-related quality of life
An expert panel judged the strength of this CUP Global evidence. There were some limitations. Still, detailed recommendations were made to strengthen future research. One of the key recommendations was for well-conducted trials to look at the impact of nutrition or physical activity. The CHALLENGE trial is therefore very timely.
The CUP Global analysis was published in the International Journal of Cancer. It was cited several times in the CHALLENGE trial manuscript.
The CUP Global analysis compared highest with lowest levels of activity. We found that all-cause mortality was reduced by 23–40% depending on physical activity exposure.
Prof Anne May, University Medical Centre, Utrecht
During our review of the literature concerning the impact of post-diagnosis physical activity on colorectal cancer prognosis for the Global Cancer Update Programme (CUP Global), we were unable to draw strong conclusions due to lacking evidence from randomized controlled trials. The Challenge trial provides exactly the evidence we were waiting for.
The summary estimate for studies that assessed activity dose was measured in MET hours per week.
- A 10 MET hour per week increase in activity was linked to a 24% reduction in all-cause mortality.
- A change of 10 MET hours per week was also the intervention goal in the CHALLENGE trial.
The effect sizes in this first, gold-standard RCT are remarkably well-aligned with the CUP Global analyses of observational studies.
During the presentation of the trial results at ASCO, the authors shared this chart. It includes the treatment benefits from approved therapies for colon, lung and breast cancer.
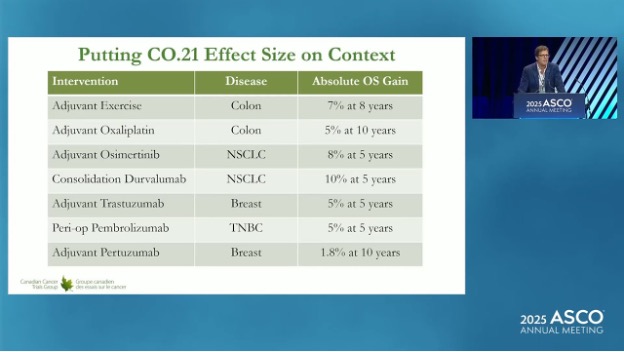
With 7–8% gains, you can see that exercise compares very favourably with other approved therapies in terms of absolute overall survival gain.
Collecting clinical trial evidence
The CHALLENGE trial confirms the clinical benefits that had been reported from observational studies. However, previous RCTs have also hinted at the accuracy of the results from observational studies. For example:
- The LEANer trial was published in 2023. It showed that triple negative breast cancer patients randomised to a diet and physical activity intervention before chemotherapy had a 53% higher rate of treatment success (eliminated cancer cells).
- A trial published in June 2025 showed that an exercise programme during and after chemotherapy increased the immune system responses in oesophageal cancer patients.
World Cancer Research Fund will fund the Optimus trial in the UK. Dr David Bartlett and Prof Adam Frampton at the University of Surrey will lead this study. It was proposed due to these findings.
Next steps
Dr Kerry Courneya co-led the CHALLENGE trial. At ASCO, he said these results could change practice for high-risk stage 2 and stage 3 colon cancer.
He expressed reservation that these results could be generalised to other sites and cancer stages. But he was optimistic that similar trials could be done more quickly than the CHALLENGE trial by taking advantage of newer methods. This could include using remote exercise assessments or activity trackers.
Dr Courneya noted that “support from funding agencies like WCRF/AICR is critical to moving this field forward because of limited access to funding for lifestyle research”.
AICR recently funded a project linked to the CHALLENGE Trial. It is led by Dr Kristin Campbell at the University of British Columbia in Canada. It will look at how muscle and fat tissue respond to exercise and how that may contribute to the observed survival benefits.
The response to the CHALLENGE Trial has made media headlines. Cancer researchers, doctors and patients are also excited by the news. This suggests that adding exercise as an additional part of treatment will gain further momentum.
While more trial data will be needed to support broader implementation, we are likely leaving the “nice to have” approach to exercise oncology and entering the “need to have” phase!
Research grants on physical activity
A selection of some of the grants we have funded that focus on the impact of physical activity on people living with and beyond a cancer diagnosis.

Prof Richard Cooke
Prof Richard Cooke is interested in what motivates people to drink alcohol – he surveys people to find out how psychological variables such as the intention to drink, attitudes about drinking, and regret after drinking alcohol – can predict how much people consume.
“Most of my research has been done with young adults aged 18–30,” says Prof Cooke, “because they were traditionally seen as the group that drinks the most, but this has changed in the last decade. I’m now doing much more research with middle-aged people. I also do studies assessing awareness of drinking guidelines, comparing how young adults and policymakers talk about alcohol, and reviewing the effectiveness of alcohol interventions.”
‘We know it’s dangerous’
“I find alcohol consumption fascinating to study as drinking has high social approval even though we know it’s dangerous. This means that health messages about alcohol are trickier to create than smoking messages. Saying ‘Don’t smoke’ is quite acceptable; saying ‘Don’t drink alcohol’ is less so,” he says.
Prof Cooke has several theories about why alcohol remains so popular across cultures: “Alcohol is a social lubricant: it relaxes people, makes them feel more confident and more able to socialise, especially with strangers. It’s really tied to our psychology in many different, sometimes unexpected, ways.”
A former student of Prof Cooke, Dr Joel Crawford, did his doctorate degree on regret and drinking. He asked young people adults about the fear of missing out (Fomo). When they don’t drink, some people think they are missing out on an enjoyable experience, like missing a party because you have to work. Dr Crawford found that the young adults would rather experience alcohol harms, such as hangovers and feeling sick, than miss events that heavily included alcohol, saying “Fomo was more painful to them than a hangover!”
This study illustrates the social and emotional barriers people trying to drink less may encounter. “It’s the social acceptability of drinking in most situations that makes it a challenge to reduce; drinking is associated with celebrations – birthdays, weddings, getting a new job, becoming a parent– and commiserations – missing out on promotion or the death of a loved one. Alcohol is also linked to healthy activities, like ending a walk in the countryside with a drink in a pub.”
Drinking’s a habit

“At the individual level, drinking habits are an issue. People develop habits when they perform the same behaviour in a stable setting, like drinking every Friday night in the pub with your friends. Breaking this habit means unpicking your routines in ways that people often don’t want to do.”
However, based on current trends, there will be fewer people drinking into middle-age and later life: “This has the potential to dramatically change how we organise events,” says Prof Cooke, comparing it to the rise in the availability and acceptability of non-dairy alternatives to milk. “People will be asking for non-alcoholic drinks at parties, and maybe that will become as acceptable as asking for an alcoholic drink is now.”
Young people prefer to stay in control
We asked Prof Cooke about why there is a decline in young people drinking alcohol. “There are several theories about why this is happening. One is that young people spend a lot of time online, and they want to present the best possible version of themselves as someone who is in control. Studies of Facebook content show that people generally share positive alcohol content, rather than negative experiences.
“Another idea is that alcohol has become more expensive in the last decade or so, which has put young people off drinking. Finally, the rise of energy drinks may be part of the explanation too, especially for young people who like to play games online. Energy drinks, high in caffeine, are likely to aid video game performance. Alcohol is unlikely to do this.”
For people of any age trying to limit their alcohol, Prof Cooke recommends trying to understand the reasons why you drink. “Do you drink to be sociable, to enhance an evening out, to cope with negative emotions? Are there other ways you could meet those needs? Psychological interventions, such as feedback on drinking or setting goals to drink less, can also be effective ways to cut back.”
Prof Cooke’s latest research
Prof Cooke’s latest research is published in Drug and Alcohol Review. He says: “Our new paper shows that policymakers and drinkers talk about drinking in different ways. While policymakers focused on drinking behaviour, drinkers talked about how drinking made them feel different emotions: embarrassed, happy, guilty, sad. Policymakers need to construct policies to reflect the importance of emotions in drinkers’ narratives.”
> Read the paper: The language of alcohol: Similarities and differences in how drinkers and policymakers frame alcohol consumption
Alcohol and cancer: let’s talk
In the UK, alcohol is a major part of how many of us socialise, relax, and celebrate. But do we really know the risks we’re taking when we drink?
Our research shows that most people don’t know that drinking any amount of alcohol increases the risk of 7 types of cancer.
This Cancer Prevention Action Week, we want to spark a national conversation: with friends, family – and within government – about alcohol and cancer.
Cancer Prevention Action Week
This year’s campaign focuses on the links between alcohol and cancer.
Research funded by World Cancer Research Fund has shown that people living with cancer who closely follow a sustainable and nutritious diet – the EAT-Lancet reference diet – have a lower risk of dying from cancer and from all causes.
This is the first study to look at the impact of the EAT-Lancet diet on people living with or beyond cancer – as opposed to the general population. Prof Sabine Rohrmann and her team at the University of Zurich, in collaboration with colleagues from another Swiss university, the UK and Austria, used UK Biobank data to see if closely following this diet – with its emphasis on eating a rich variety of plant foods – affected the risk of death for people with a cancer diagnosis at the time they were recruited for the study.
Studying more than 25,000 people with an average age of 60 years at recruitment, the researchers used dietary information collected in the UK Biobank to develop a score that reflected how closely participants followed the EAT-Lancet diet.
More support needed for people facing cancer
Of the 25,348 cancer survivors in the group studied, 4,781 people died during the study follow-up. Prof Rohrmann’s results showed modest links between closely following the diet and a lower risk of dying from cancer, and of dying from all causes. The researchers didn’t observe a link between the diet and dying from heart disease.
Almost 64% of the participants were female, and participants who followed the EAT-Lancet diet more closely were more likely to be female. However, this study confirmed previous evidence showing that people living with and beyond cancer do not tend to follow healthy diets after their diagnosis. This emphasises the need to help people form healthier habits and overcome the barriers to eating well, such as treatment side-effects affecting appetite and taste.
These findings highlight the importance of greater nutrition support and guidance for people facing cancer. Guidelines aimed at the general population are unlikely to consider the needs of people living with and beyond cancer. With a lack of evidence-based recommendations for this population, the gap can sometimes be filled by practices not supported by the science – such as excessive use of dietary supplements.
This evidence showing the benefits of the EAT-Lancet diet follows recent research by our Global Cancer Update Programme, which provided guidance for people with a breast or a bowel cancer diagnosis.
Prof Sabine Rohrmann
We specifically put the focus of our study on cancer survivors because we believe that it is important to encourage them to follow a healthy lifestyle. For this, we need more evidence and so far, research on lifestyle changes in cancer survivors is still scarce.
Dr Julia Panina, Head of Research Funding
This study provides important new evidence that following the EAT-Lancet reference diet may reduce the risk of mortality in people living with and beyond cancer. The focus on the consumption of plant-based foods reflects our Cancer Prevention Recommendations to eat more wholegrains, vegetables, fruit and beans, and to limit red and processed meat. Importantly, these findings also show that diets supporting cancer survivorship can promote more sustainable eating and help protect the environment.
The EAT-Lancet reference diet was created by a team of scientists (The EAT-Lancet Commission on Food, Planet, Health) in 2019. It is a mainly plant-based diet that, according to the Commission, addresses the environmental impact of food production and consumption better than most national dietary guidelines.
> Read the paper: Higher adherence to the EAT-Lancet reference diet is inversely associated with mortality in a UK population of cancer survivors
> On the blog: Plant-based diets: eating for our health and the planet
Researchers funded by World Cancer Research Fund have discovered that brisk walking is linked to a lower risk of 5 cancers:
- anal
- liver (hepatocellular carcinoma)
- small intestine
- thyroid
- lung
Using information stored in the UK Biobank – a large database of many different aspects of health – scientists explored the link between walking pace – slow, steady or brisk – and the risk of developing 28 types of cancer.
They confirmed that the link between brisk walking and a reduced risk of developing the 5 cancers was true, even after accounting for overall physical activity and total walking time.
Speeding up your walk could represent an easy, low-cost public health intervention to decrease cancer risk.
The paper, published in BMC Cancer, says:
“Adopting a brisk walking pace may represent a pragmatic target for public health interventions to decrease cancer risk, particularly in circumstances where increases in walking volume or frequency prove impractical.”
PhD student Michael Stein’s research was supported by funding from Prof Michael Leitzmann’s grant. This research was funded by World Cancer Research Fund as part of the WCRF International Regular Grant Programme.
> Read the full paper: Usual walking Pace and risk of 28 cancers– results from the UK biobank
Our research portfolio spans a wide range of areas within cancer prevention. Today we’re spotlighting a lab-based study taking place in Newcastle. Local MP Chi Onwurah met Assoc Professor Jill McKay, Prof Dianne Ford and Dr Jessica Saville from Northumbria University, to discuss their groundbreaking cancer prevention research.
Hosted at the university, Chi learned about cancer prevention at the molecular level through her engagement with Assoc Prof Jill McKay and her team. World Cancer Research Fund awarded the team a £347,000 grant to conduct a laboratory-based study investigating whether folate levels in expectant mothers are linked to the development of leukaemia in their children. Folate is a B-vitamin naturally found in green leafy vegetables and liver, while its synthetic form, folic acid, is commonly used in supplements and fortified foods. Some studies suggest folic acid supplementation during pregnancy may help prevent childhood leukaemia; however, findings are not yet clear.
Leukaemia, a cancer of the blood, is the most common childhood cancer worldwide, responsible for 1 in 3 childhood cancers, and rates are slowly increasing. This important research could identify biological markers to help screen or monitor children at increased risk. Ultimately this could lead to earlier diagnosis, which is closely tied to better outcomes for leukaemia patients. It could also result in improved nutritional guidelines for pregnancy.
Assoc Prof Jill McKay, Principal investigator, Northumbria University
Rates of childhood leukaemia are slowly rising, which suggests some things in our environment may be contributing to this disease developing. Learning more about what factors can affect leukaemia and how they influence underlying biology can help us know which lifestyle changes we can make to aim to prevent and predict childhood leukaemia. However, none of this will be possible unless we liaise with policy makers, so we are delighted to meet with Chi today to share our exciting research.
Importantly, the researchers and MP discussed the study’s potential to influence nutritional guidelines during pregnancy, reduce the risk of childhood leukaemia, and support earlier diagnosis. As Chair of the Science, Innovation and Technology Committee, Chi Onwurah MP was particularly interested in hearing about the study’s progress, upcoming publications, and future plans following its completion.
Dr Jana Sremanakova, Research Funding Manager, WCRF International
This is a particularly exciting and important moment for us at the World Cancer Research Fund, as it marks the first time we are connecting our grant holders directly with their MP. It’s a unique opportunity to highlight the impact of our work in cancer prevention research and our national cancer prevention efforts.
Despite the advances in cancer research over the past 40 years, including World Cancer Research Fund’s evidence on cancer prevention, and dramatic advances in cancer treatment, one question remains to be answered: why does one person get cancer when another, who lives a similar lifestyle, does not?
Experts estimate that up to 40% of cancer cases are preventable, if people didn’t smoke, avoided the sun, avoided alcohol, ate a healthy diet, maintained a healthy body weight and stayed physically active. But that doesn’t mean we can reduce our own risk of cancer by 40% if we follow this advice. It’s not easy to estimate an individual’s cancer risk because so many biological and genetic factors are also at play.
And that’s where large databases about our health can make a big difference. One of these is the UK Biobank, which contains details about the health – and increasingly, as the participants get older, the ill-health, of 500,000 people in the UK. The longevity of this data – not just at one point in a person’s life but repeatedly measured over a long period of time – helps us understand what influences cancer risk throughout someone’s life.
Heel bone density to house size
Since 2006, the UK Biobank has been collecting environmental, lifestyle and genetic information about the participants. For scientists, the size, range of information – from heel bone density to blood pressure to the size of their house – and duration of information collected is a gold mine.
It has been described as “the world’s most important health database” yet it’s not the only resource of this type. Another large database established as part of the European Prospective Investigation into Cancer and Nutrition (EPIC) study has grown into a massive project involving 10 countries, with 521,000 participants and data collected over more than 30 years.
Of the 30,000 registered researchers from 100 countries who have used data from the UK Biobank, some are funded by the World Cancer Research Fund network, and are using the data to investigate a range of cancer risk factors:
- Sleep, sleep patterns, and risk of prostate and endometrial cancer
- Fat tissue and advanced prostate cancer risk
- Social inequality and cancer risk
- Physical activity, sedentary behaviours, and cancer, cardiovascular disease and diabetes
- Plant-based diets
- Ultra-processed food
- Following our Cancer Prevention Recommendations
- Obesity and insulin
- Vegetarian diets
- Links between diabetes and cancer
- How many cancers are linked to obesity and physical activity?
Some of the things our scientists have found out using UK Biobank data include:
- Physical activity across the day – with a peak early in the morning and late in the evening – linked to lower risk of colorectal cancer
- Ultra-processed food increases cancer risk
- Following our Cancer Prevention Recommendations reduces the risk of all cancers
The UK Biobank allows researchers around the world to look at biological and medical data and “supports a diverse range of research intended to improve the prevention, diagnosis and treatment of illness, and the promotion of health throughout society”.
And it’s not easy to get hold of such large amounts of data. It’s hard to get half a million people to consent to sharing their personal data in this way, and even harder to get them to keep filling in surveys and undergoing procedures over many years. This type of research can only be done with people’s support and willingness to consent, and without it, finding ways to prevent and treat diseases such as cancer will be so much harder.
The wealth of data the UK Biobank contains could have drastic implications for cancer research, perhaps even finally helping realise World Cancer Research Fund’s ambition of living in a world where no one dies of a preventable cancer.
What do our grant holders say about UK Biobank?
Prof John Mathers
The scale, rich detail of participant characteristics and behaviours, and robust long-term information on health outcomes make UK Biobank a world-leading resource for studies of many aspects of nutrition and health including cancer risk and survival.
Dr Emma Allott
Whole body imaging data available in UK Biobank has enabled our team to measure the amount of fat surrounding the prostate in a large number of cancer-free men. These men are followed over time by the UK Biobank, giving us the opportunity to explore how the quantity of this fat type is related to future risk of prostate cancer. Studies like UK Biobank are critical for this type of research as the imaging required to measure this fat type is not otherwise available in healthy individuals. The results of our study will provide the first evidence for or against periprostatic fat as a risk factor for aggressive prostate cancer.
Dr Dagfinn Aune
We are using the UK Biobank to study the association between adiposity and physical activity and cancer risk. The very large sample size and the detailed assessment of adiposity measures, physical activity, other risk factors and a range of biomarkers are of major importance for our analyses. All this information helps us study associations with a range of cancer outcomes as well as exploring potential biological mechanisms that may explain or contribute to cancer development.
Dr Fiona Malcomson
Our studies using UK Biobank data have shown that people who adhere more closely to the WCRF/ AICR Cancer Prevention Recommendations have lower risk of developing cancer and, specifically, lower risk of cancer of the breast, bowel, kidney, oesophagus, ovary, liver and gallbladder. UK Biobank data has also enabled us to identify lifestyle and dietary patterns according to sociodemographic factors that will help guide public health strategies for cancer prevention.
Eating a wide variety of food may reduce the risk of gastrointestinal cancers, according to research funded by the World Cancer Research Fund network* and published in the European Journal of Cancer.
Little is known about how eating a wide variety of food species, also known as food biodiversity, may benefit our health or affect our cancer risk. Food species refer to a distinct type of plant or animal, such as wheat, chicken, or salmon. For example, salmon, mackerel, and tuna are all separate food species, even though they share some biological traits and belong to the same food group. Similarly, rocket, lettuce and spinach count as separate food species, even though they are all leafy green vegetables. However, chicken and a chicken’s egg belong to the same food species even though they are different types of food.
This study is the first to examine how the number of different food types consumed, measured as Dietary Species Richness (the number of species an individual consumes per year) affects the risk of the following gastrointestinal cancers:
- Oesophagus
- Throat
- Stomach
- Bowel
- Colon
- Rectum
- Gallbladder
- Pancreas
- Liver
The study followed 450,111 cancer-free adults in 9 European countries from the European Prospective Investigation into Cancer and Nutrition cohort for 14 years. The researchers, from the International Agency for Research on Cancer, found that individuals with the most diverse diets, by including more food species in their diet, had a 23% lower risk of developing gastrointestinal cancers compared with those with the least variety. The risk decreased by 6% for every 10 extra species per year added to their diet. People can do this by including more variety in the types of fruit and vegetables they eat, for example, choosing to eat local and seasonal fruit and vegetables of different colours.
Food biodiversity includes eating different types of food that provide the necessary nutrients for maintaining health. Investigating food biodiversity is important because it has the potential to benefit public health and sustainable food systems.
Dr Helen Croker, our Assistant Director of Research and Policy, said: “Diets have become more limited in the types of foods eaten and they are often high in fat, sugar and salt. However, for cancer prevention, it’s important to eat a healthy, balanced and varied diet with plenty of wholegrains, pulses, vegetables and fruit.”
Dr Helen Croker
This study is particularly interesting because it looks at the number of different foods people eat and the impact it can have on their cancer risk, in particular gastrointestinal cancers. More research is now needed to confirm these findings and further explore the link between dietary diversity and cancer prevention.
Dr Inge Huybrechts
This study shows how a more diverse diet, including a large variety of species, could lower the risk of gastrointestinal cancers, emphasising the importance of eating a wide variety of foods. The idea behind a diverse diet consisting of many types of plants and animals species may provide essential nutrients for the body while also strengthening ecosystems, making them more resilient, productive, and sustainable.
Another study from this grant looked at how food biodiversity is measured. Methods such as Hill numbers estimate the number of species, but it wasn’t clear whether these numbers could be compared across different study settings.
The findings showed that Dietary Species Richness is the most feasible way to measure and evaluate food biodiversity across various contexts, and considering high-, middle- and low-income countries. Regardless of which Hill number was used, however, all measures indicated that greater food biodiversity was associated with better micronutrient sufficiency and with lower rates of all-cause mortality, this latter association yet being strongest for Dietary Species Richness.
This grant was funded by Wereld Kanker Onderzoek Fonds based in the Netherlands, as part of the World Cancer Research Fund International network.
> More on this grant: Will a balanced diet also save the planet?










