Research funded by Wereld Kanker Onderzoek Fonds (WKOF), as part of the World Cancer Research Fund International grant programme, has produced evidence strengthening the case that higher alcohol intake increases bowel (colorectal) cancer risk across its different tumour subtypes. It is the largest ever study on that topic.
It is already well known that drinking alcohol increases the risk of bowel cancer, but the mechanisms needed to be better understood.
Now, the researchers led by Dr Christos Chalitsios and Dr Konstantinos Tsilidis at the University of Ioannina (Greece) and Imperial College London (UK) and the University of Ioannina (Greece), working with international consortia, have brought clearer answers to one of the most important long-standing questions: when alcohol increases bowel cancer risk, does it do so mainly through particular “molecular pathways” of the disease, or broadly across them all?
Looking across cancer pathways
To investigate this, researchers pooled data from large consortia (GECCO and the Colon Cancer Family Registry), analysing more than 22,000 people (11,826 cases and 10,888 controls).
Because bowel cancers aren’t all the same, the team examined tumour subtypes defined by molecular features including microsatellite instability (MSI), CpG island methylator phenotype (CIMP), and mutations in the BRAF and KRAS genes.
The key finding was that the alcohol–cancer association looked broadly similar across MSI, CIMP, BRAF and KRAS tumour subtypes (and in combined “pathway” groupings).
In other words, the study found no convincing evidence that alcohol preferentially drives one major molecular subtype over another.
Higher intake, higher risk
Among people who drink alcohol, risk increased with higher intake: each additional 14 g/day (about 1 drink/day) was linked with around a 10% higher colorectal cancer risk, and this pattern was mainly driven by heavier drinking (more than 28 g/day, roughly more than 2 drinks/day).
Genetic analyses further supported a link between higher alcohol consumption and higher overall colorectal cancer risk, and again did not suggest that risk is confined to any single subtype.
What this means for cancer prevention is clear. Heavier drinking appears to increase bowel cancer risk regardless of tumour subtype. Therefore, our recommendation for cancer prevention continues to be to avoid alcohol. If you do drink, cutting down can help reduce your risk, because there is no completely safe level of alcohol intake when it comes to cancer.
Dr Tsilidis explained:
“Alcohol is consistently associated with a range of adverse health outcomes, and contemporary evidence no longer supports the idea that it is “good” for health at any level. Although there are still unknowns in alcohol and health research, alcohol should not be recommended for disease prevention, and people who choose to drink are advised to keep consumption as low as possible.”
To celebrate Cancer Prevention Action Week and to kickstart summer, we’ve pulled together our favourite mocktail and alcohol-free drink recipes, which are perfect for events from parties to BBQs, day or evening.
Did you know that drinking alcohol increases your risk of 7 types of cancer, including breast and bowel?
Alcoholic drink can also have a lot of hidden calories. Reducing how much alcohol you drink may support weight management, which in turn can help lower your risk of cancer. Unlike many alcohol-free drinks you find in a shop or pub, our mocktail recipes are all lower in calories with no added sugar.
Our top 7

Alcohol-free G&T
Enjoy the crisp tones in our no-alcohol gin and tonic, with a grapefruit twist for something different this summer.
⏰ 5 minutes
🍎 1 of 5 A DAY
🧍♂️ serves 2
 Berry sparkle
Berry sparkle
For a healthy alternative to prosecco, our refreshing berry fizz is a perfect option, and so easy to make.
⏰ 5 minutes
🧍♂️ serves 2

Pink lemonade
A family favourite, our rose-blueberry lemonade is a great addition to any BBQ.
⏰ 5 minutes
🧍♂️ serves 2
 Watermelon slushie
Watermelon slushie
Enjoy the tangy notes of watermelon, raspberries and lime with this healthy slushie.
⏰ 10 minutes
🍎 1 of 5 A DAY
🧍♂️ serves 2
 Peach iced tea
Peach iced tea
In warmer weather, a hot cup of a tea isn’t always the best, so this peach iced tea is a refreshing alternative to enjoy during the summer months.
⏰ 10 minutes plus cooling
🍎 Less than 1 of 5 A DAY
🧍♂️ serves 8
 Cucumber cooler
Cucumber cooler
Refresh yourself on dry days with a summery cucumber cooler that kids will love.
⏰ 5 minutes
🧍♂️ Serves 2
> Get the recipe
On the blog
As part of Cancer Prevention Action Week 2025, on Wednesday we handed in an open letter and petition, alongside breast cancer survivors Dr Liz O’Riordan and Nikki Bednall, and the Alcohol Health Alliance.
The letter (below) – signed by more than 25 organisations and health experts – and the petition called on Prime Minister Sir Keir Starmer and his government to introduce a National Alcohol Strategy to Prevent Cancer, as part of our Cancer Prevention Action Week (CPAW) activity.
This year, CPAW is highlighting the links between alcohol and cancer – our research shows that most people don’t know that drinking any amount of alcohol increases the risk of 7 types of cancer.
What’s more, around 17,000 new cases every year are down to alcohol – so we’re urging the UK government to introduce a long-overdue National Alcohol Strategy for England – one that tackles alcohol harm head-on through:
- mandatory health warnings highlighting cancer risk
- minimum unit pricing
- marketing restrictions
to reduce consumption, lower cancer risk, and protect lives.





Read the full letter below
The Rt Hon Keir Starmer MP
Prime Minister
10 Downing Street
London SW1A 2AA
CC: The Rt Hon Wes Streeting MP, Secretary of State for Health and Social Care
Ashley Dalton MP, Parliamentary Under-Secretary of State for Public Health and Prevention
25 June 2025
The UK government must act on alcohol now to prevent cancer
Dear Prime Minister,
On behalf of more than 20 organisations and public health leaders, we are writing to share our deep concern about the continued lack of action to reduce alcohol consumption across the United Kingdom. In particular, the absence of a National Alcohol Strategy for England stands in stark contrast to the scale of harm caused by alcohol, with alcohol-specific deaths having increased by 42% in England between 2019 and 2023 alone.
This week marks Cancer Prevention Action Week (CPAW) – a national campaign led by World Cancer Research Fund (WCRF) – which seeks to empower the public and inspire change to prevent cancer. This year, CPAW is shining a spotlight on the link between alcohol and cancer, and the urgent need for government action.
In the UK, alcohol causes around 17,000 cases of cancer every year – equivalent to 46 people receiving a diagnosis every single day. And as our population ages and grows, these numbers are projected to rise. Worryingly, the pandemic has also driven an increase in high-risk drinking. Modelling by the Institute of Alcohol Studies and Health Lumen suggests that if this trend persists, we could see an additional 18,785 cancer cases by 2035.
Public awareness remains alarmingly low that alcohol is a Group 1 carcinogen, the same category as tobacco and asbestos, and a cause of seven types of cancer, including two of the most common breast and bowel as well as mouth and throat, oesophageal, liver and stomach cancer. These risks are present even at low levels of consumption. New polling commissioned by WCRF reveals that when asked unprompted only 1 in 14 UK adults are aware that alcohol increases cancer risk and 25% believe there is no health risk attached to drinking alcohol.
We are not alone in our concern – thousands of members of the public including more than 20 organisations have signed our petition calling for greater government action. They agree that no one should have to suffer the devastating trauma of alcohol-related cancer.
The human toll is compounded by the economic burden. In 2016, Cancer Research UK estimated that alcohol-attributed cancers cost the NHS alone an estimated £100 million annually. With the health service under immense strain, it is imperative to act now and realise the government’s priority of prevention.
Despite alcohol being the sixth leading cause of preventable cancer in the UK, current policy does not reflect this reality. We urge the government to fulfil its responsibility to protect public health by introducing a National Alcohol Strategy for England without delay, which must include:
- Mandatory alcohol product labelling with health warnings, including information on cancer risks and calorie content.
- Marketing restrictions on alcohol by classifying it as an ‘unhealthy product’ under high fat, salt and sugar marketing restrictions.
- Implementing and evaluating minimum unit pricing at 65p in England with rates adjusted in line with inflation, to bring England into line with Scotland, Wales and Northern Ireland who all either have MUP already or have stated their intention to implement.
It is vital that this strategy aligns with the forthcoming National Cancer Plan for England, ensuring that alcohol is comprehensively addressed as a modifiable risk factor for cancer. We also urge the UK government to work in close collaboration with the devolved administrations, particularly to enable action to improve approaches to labelling and advertising. All policy development processes must be protected from industry influence and vested interests to ensure public health is placed above profit.
Such action would not only help to reduce cancer risks but reduce other alcohol-related harms. It would also support the government’s own ambitions to shift from sickness to prevention, as set out in the Health Mission, and contribute to economic growth by reducing illness-related inactivity.
We stand ready to support this effort and urge you to act now. Together we can tackle the devastating impact of both alcohol harm and cancer.
Yours sincerely,
Rachael Gormley, Chief Executive, World Cancer Research Fund
Dr Richard Piper, CEO, Alcohol Change UK
Alison Douglas, Chief Executive, Alcohol Focus Scotland
Professor Sir Ian Gilmore, Chair, Alcohol Health Alliance
Greg Fell, President, Association of Directors of Public Health
Dr Heather Grimbaldeston, Chair, BMA Public Health Medicine Committee, British Medical Association
Professor David Strain, Chair, BMA Board of Science, British Medical Association
Thalie Martini, Chief Executive Officer, Breast Cancer UK
Eddie Crouch, Chair, British Dental Association
Pamela Healy OBE, Chief Executive, British Liver Trust
Jill Clark, Chair, CancerWatch
Alison Wise, Communications Manager, on behalf of Fight Bladder Cancer
Ailsa Rutter OBE, Director, Fresh and Balance
Kostas Tsilidis, Associate Professor of Cancer Epidemiology and Prevention, Imperial College London
Dr Katherine Severi, Chief Executive, Institute of Alcohol Studies
Dr Dominique Florin, Medical Director, Medical Council on Alcohol
Daniela Binnington Nessman, Founder, Menopause and Cancer
Gopika Chandratheva, Nutritionist, NHS
Tamara Khan, CEO, Oracle Head & Neck Cancer UK
Jon Coleman-Reed, Head of Operations, Prevent Breast Cancer
Dr Claire Shannon, President, Royal College of Anaesthetists
Robert Steele, Chair, Board Directors, Scottish Cancer Foundation
Dr Alastair MacGilchrist, Chair, Scottish Health Action on Alcohol Problems
Chris Curtis, Chief Executive Officer, Swallows Head & Neck Cancer Support Charity
Amandine Garde, Professor of Law & Non-Communicable Diseases Research Unit, University of Liverpool
Richard Cooke, Professor of Health Psychology, University of Staffordshire
Dr Kathryn Scott, Chief Executive, Yorkshire Cancer Research
‘Who Comes Here?’, ‘A Grenadier’ – Victorian nursery rhyme illustration (Getty Images). From “Nursery Rhymes – Ridicula Rediviva” illustrated by J.E. Rogers, with chromolith printing by R. Clay Sons & Taylor and published in London in 1876 by Macmillan and Co.
World Cancer Research Fund has been highlighting the links between alcohol and cancer for more than 30 years – but we weren’t the first to do this.
In fact, as Britain recovered after the First World War, beer producers launched campaigns to get people – especially men and boys – back into the pub, with slogans such as “Guinness is good for you” and “Beer is best”. Yet this move by beer makers was a reaction to the thriving temperance movement, which fought back with postcards that said: “Beer is best – for cancer”, listing the cancers alcohol was associated with including brain and mouth.
This is just one aspect of the long history of drinking – and sobriety – in Britain. Did people really drink beer because water was unsafe? Why did people turn to gin? And was Irn-Bru an original tipple of choice for teetotallers? Read on to find out.
Small beer gets bigger
We know through archaeological deposits that people have been drinking beer for around 13,000 years. Beer has certainly been an important drink – especially for poorer people – in the UK for more than 1,000 years. In the Medieval era (around 5th–15th centuries), beer was not just a staple drink. It was also a vital source of calories. At that time, beer and ale were graded according to how long the liquid had been fermented, its strength and the quality of the ingredients. “Small beer” was the weakest and most widely drunk option. Prof Phil Withington of the University of Sheffield says: “Small beer was an integral feature of British diets and was drunk at all times of the day from breakfast.”

A man dressed up as a medieval monk pours himself some beer. Getty Images
However, it’s not true that everyone had to drink beer because the water was unsafe. Most people at this time would have lived in rural areas, and local rivers and streams would have been a source of drinking water. Both beer and ale were safer than some water sources, though, because they are heated during production.
A major change in Britain’s drinking habits occurred in the 1700s onwards with the arrival of gin – dead cheap and often home brewed – which coincided with the start of the industrial revolution, when people moved on mass from rural, family dwellings to less sanitary urban and suburban areas. The pub became a respite for people after working long hours in factories and provided an escape from cramped multi-generational living conditions. “Drink was everywhere; it was economically important and culturally unavoidable,” Dr David Beckingham told History Extra.

Antique advertisement from British magazine: Dinner wine
Gin sends Britain wild
Gin was widely available, low-taxed and – incredibly – sold in pints as people were accustomed to drinking beer in pints. Gin is distilled rather than fermented – which means it’s a lot stronger. Stories we’re familiar with today – around binge drinking, the social impact of alcohol harm (especially when women and poorer people drink to excess), and attempts to curb drinking through public pressure, moral panics and legislation – all began with the Gin Craze. Then as now, alcohol had a class element, with the wine and champagne drunk by the rich seen as less damaging to society and health than the beer and gin of the poor.
And today’s sober curious movement has its history in the anti-drink movements that started at this time. Initially, the backlash against gin focused on temperance – encouraging people to limit their alcohol consumption, mainly by drinking weaker but still alcoholic drinks. The 1830 Beerhouse Act allowed people to brew beer from home – an attempt to reduce gin drinking. However, some strands of the movement favoured total abstinence.
The Band of Hope, established in 1847, became the biggest temperance organisation in Britain, with 3.5 million members by the end of the 19th century. It was a youth-led movement, and part of the attraction was that it offered young people an (often cheaper) alternative to the pub. As well as pressurising members with signed pledges, badges and magazines, temperance societies organised fun stuff: brass bands, sober cafes, music hall events and outings. The first temperance day trip was an excursion from Leicester to Loughborough in 1841, for 500 temperance society members. The man who arranged it was none other than Thomas Cook – the inventor of package holidays.
So what alcohol-free drinks were around in the 18th and 19th centuries? Initially, most concoctions were mixes of readily available herbs and water, often heavily sweetened: sarsaparilla “wine”, dandelion and burdock, cream soda and ginger beer – as well as tea. Some of the biggest brands in soft drinks also emerged at this time. Teetotallers drank fortifying iron brew (later Irn Bru), Coca-Cola and Vim Tonic, as well as milk drinks – precursors of today’s milkshake and bubble tea bars.
It wasn’t plain sailing for those trying to cut back on alcohol though. The temptations of alcohol versus the guilt of overindulgence are revealed in the diaries (written between 1830 and 1881) of Nottingham solicitor and mayor William Parsons, who talks about his attempts to go dry in January, and how hard it was to avoid booze in social gatherings: “Tea totalism in my position is not carried out without great difficulty.”
As well as persuading individuals to change their drinking habits, people who advocated for drink-free living leaned on politicians to legislate for restrictions on the sale of alcohol, and taxation to reduce its availability and affordability. The fact that we’re trying the same approaches hundreds of years later shows the difficulty of breaking up Britain’s relationship with the booze.
Temperance as a movement died off from the 1950s as alcohol became even more widely marketed and socially acceptable. This is perhaps reflected in the licensing changes. Since 1988, pubs have been able to open all day and 24-hour licensing was introduced in 2005. Despite this, younger generations seem to be drinking less than their elders. In England’s 2022 health survey, the highest prevalence of drinking on at least 1 day a week was among adults aged 65–74, whereas the lowest was among 16–24-year-olds (60% vs 36%).
Our theme for Cancer Prevention Action Week is Alcohol and cancer: let’s talk. The UK’s long history of drinking – and staying sober – shows that alcohol is deeply embedded in British society. Yet even though we’re no longer in the midst of a gin craze, the harms of alcohol are widespread. As those abstinence campaigners at the start of the last century knew, alcohol is a cancer-causing, psychoactive, toxic, and dependence-producing substance linked to more than 200 health conditions. Everyone deserves to know the history – and the truth – about alcohol.

Prof Richard Cooke
Prof Richard Cooke is interested in what motivates people to drink alcohol – he surveys people to find out how psychological variables such as the intention to drink, attitudes about drinking, and regret after drinking alcohol – can predict how much people consume.
“Most of my research has been done with young adults aged 18–30,” says Prof Cooke, “because they were traditionally seen as the group that drinks the most, but this has changed in the last decade. I’m now doing much more research with middle-aged people. I also do studies assessing awareness of drinking guidelines, comparing how young adults and policymakers talk about alcohol, and reviewing the effectiveness of alcohol interventions.”
‘We know it’s dangerous’
“I find alcohol consumption fascinating to study as drinking has high social approval even though we know it’s dangerous. This means that health messages about alcohol are trickier to create than smoking messages. Saying ‘Don’t smoke’ is quite acceptable; saying ‘Don’t drink alcohol’ is less so,” he says.
Prof Cooke has several theories about why alcohol remains so popular across cultures: “Alcohol is a social lubricant: it relaxes people, makes them feel more confident and more able to socialise, especially with strangers. It’s really tied to our psychology in many different, sometimes unexpected, ways.”
A former student of Prof Cooke, Dr Joel Crawford, did his doctorate degree on regret and drinking. He asked young people adults about the fear of missing out (Fomo). When they don’t drink, some people think they are missing out on an enjoyable experience, like missing a party because you have to work. Dr Crawford found that the young adults would rather experience alcohol harms, such as hangovers and feeling sick, than miss events that heavily included alcohol, saying “Fomo was more painful to them than a hangover!”
This study illustrates the social and emotional barriers people trying to drink less may encounter. “It’s the social acceptability of drinking in most situations that makes it a challenge to reduce; drinking is associated with celebrations – birthdays, weddings, getting a new job, becoming a parent– and commiserations – missing out on promotion or the death of a loved one. Alcohol is also linked to healthy activities, like ending a walk in the countryside with a drink in a pub.”
Drinking’s a habit

“At the individual level, drinking habits are an issue. People develop habits when they perform the same behaviour in a stable setting, like drinking every Friday night in the pub with your friends. Breaking this habit means unpicking your routines in ways that people often don’t want to do.”
However, based on current trends, there will be fewer people drinking into middle-age and later life: “This has the potential to dramatically change how we organise events,” says Prof Cooke, comparing it to the rise in the availability and acceptability of non-dairy alternatives to milk. “People will be asking for non-alcoholic drinks at parties, and maybe that will become as acceptable as asking for an alcoholic drink is now.”
Young people prefer to stay in control
We asked Prof Cooke about why there is a decline in young people drinking alcohol. “There are several theories about why this is happening. One is that young people spend a lot of time online, and they want to present the best possible version of themselves as someone who is in control. Studies of Facebook content show that people generally share positive alcohol content, rather than negative experiences.
“Another idea is that alcohol has become more expensive in the last decade or so, which has put young people off drinking. Finally, the rise of energy drinks may be part of the explanation too, especially for young people who like to play games online. Energy drinks, high in caffeine, are likely to aid video game performance. Alcohol is unlikely to do this.”
For people of any age trying to limit their alcohol, Prof Cooke recommends trying to understand the reasons why you drink. “Do you drink to be sociable, to enhance an evening out, to cope with negative emotions? Are there other ways you could meet those needs? Psychological interventions, such as feedback on drinking or setting goals to drink less, can also be effective ways to cut back.”
Prof Cooke’s latest research
Prof Cooke’s latest research is published in Drug and Alcohol Review. He says: “Our new paper shows that policymakers and drinkers talk about drinking in different ways. While policymakers focused on drinking behaviour, drinkers talked about how drinking made them feel different emotions: embarrassed, happy, guilty, sad. Policymakers need to construct policies to reflect the importance of emotions in drinkers’ narratives.”
> Read the paper: The language of alcohol: Similarities and differences in how drinkers and policymakers frame alcohol consumption
Alcohol and cancer: let’s talk
In the UK, alcohol is a major part of how many of us socialise, relax, and celebrate. But do we really know the risks we’re taking when we drink?
Our research shows that most people don’t know that drinking any amount of alcohol increases the risk of 7 types of cancer.
This Cancer Prevention Action Week, we want to spark a national conversation: with friends, family – and within government – about alcohol and cancer.
Cancer Prevention Action Week
This year’s campaign focuses on the links between alcohol and cancer.
Only 16% of us in the UK feel at ease discussing our relationship with alcohol, ranking it among the least talked about topics – less so than sex (17%) and money (29%), according to our poll.
We’re emphasising the connection between alcohol and cancer as part of Cancer Prevention Action Week, which starts today. We have strong evidence that alcohol increases the risk of 7 cancers:
- Breast
- Bowel
- Head and neck
- Oesophageal
- Liver
- Stomach
Alcoholic drinks are also high in calories and often high in sugar, increasing the risk of gaining weight. Living with overweight or obesity increases the risk of at least 13 types of cancer.
We surveyed 2,000 people to gain insights into Britain’s understanding of alcohol and cancer risks. The findings reveal consistent misconceptions regarding alcohol’s dangers. Alarmingly, 25% of respondents did not associate any health risks with alcohol, and only 1 in 14 mentioned cancers as a risk when asked unprompted.
These misconceptions may hinder our ability to have informed conversations about alcohol. About 4% of cancer cases in the UK are attributed to alcohol, meaning that, each year, around 17,000 people are diagnosed with cancer caused by alcohol. Adding to this immeasurable human cost is the economic burden. Alcohol-related cancers cost the NHS around £100m every year.
We need a National Alcohol Strategy
We support clearer public health messaging to raise awareness of the real dangers of alcohol consumption, as well as other measures such as health warning labels. Alongside many other health organisations in the UK, we’re urging the Prime Minister, Sir Keir Starmer, to implement a National Alcohol Strategy for England.
World Cancer Research Fund CEO Rachael Gormley
Alcohol is pervasive in our lives, from celebrations to after-work drinks. But do we truly understand the risks involved? It’s essential that we engage in more discussions about alcohol and cancer, empowering individuals to make informed health choices.
Alcohol Health Alliance Chair Sir Ian Gilmore
One of the reasons public awareness is so low is that we're being kept in the dark about the true cost of drinking. People have the right to know the full picture so that they can make informed choices about what they consume.
World Cancer Research Fund Executive Director of Research and Policy Dr Giota Mitrou
A long-overdue National Alcohol Strategy in England would help the government tackle alcohol harm head on – reducing consumption, lowering cancer risk, and protecting lives.
Nikki Bednall is a World Cancer Research Fund Supporter and breast cancer survivor. She said: “I always thought drinking a few times a week was fine. I never knew it could raise my cancer risk. If I’d known earlier, I might have made different choices. Though hindsight is easy, my perspective has changed with the knowledge that came after my diagnosis.”
Drinking habits in the UK paint a concerning picture in comparison with other nations. Organisation for Economic Cooperation and Development (OECD) 2021 data showed that alcohol consumption in the UK was 10 litres per capita – 16% more than the OECD average of 8.6 litres.
Covid led to an increase in the number of high-risk drinks, with the heaviest drinkers increasing their consumption the most. These changes have persisted beyond the national lockdowns of 2020 and 2021, and subsequently there has been a year-on-year rise in alcohol-specific deaths, which reached an all-time high of 10,473 in 2023.
The research was conducted by Opinion Matters, among a sample of 2,000 nationally representative UK adults. The data was collected between 21.03.2025–24.03.2025.
Cancer Prevention Action Week (CPAW)
This year we’re highlighting the links between alcohol and cancer.
Alcohol and cancer: let’s talk – that was the theme of this year’s Cancer Prevention Action Week. For 7 days on 23–29 June, we talked to politicians, gave radio interviews and spoke to experts about alcohol and cancer. Plus, we shared news and views across our socials:
Facebook | LinkedIn | Instagram | Bluesky
How Cancer Prevention Action Week unfolded
Monday’s highlights
> Brits find it harder to talk about alcohol than sex or money
Yorkshire GP speaks out in support of CPAW:
Dr Nigel Wells, Medical Director and Executive Director Clinical & Care Professional Humber and North Yorkshire ICB and practising GP:
As a GP, I know people can be reluctant to talk about alcohol or share concerns about their drinking – so it doesn’t surprise me that only 2 in 10 people across Yorkshire and the Humber feel comfortable doing so.
But alcohol isn’t harmless – it increases the risk of 7 types of cancer, and, too often, people simply aren’t aware. If this campaign helps someone pause and ask whether alcohol might be affecting their health, and encourages them to speak to a healthcare professional, it will have made a real difference. We need to make these conversations as routine as those about smoking or diet – and that starts with creating a safe, non-judgemental space in every consultation.
We tabled an Early Day Motion in support of Cancer Prevention Action Week. And Alcohol Focus Scotland, a key supporter of this year’s campaign, tabled a motion in the Scottish Parliament on alcohol and cancer.
Tuesday’s highlights

Alcohol Focus Scotland organised a photo call at Holyrood with Members of the Scottish Parliament (MSPs). Photographed are 11 MSPs, including the Cabinet Secretary for Health Neil Gray; Jackie Baillie, Labour’s deputy leader and health spokesperson, and Presiding officer Alison Johnstone. Read more on LinkedIn
Sheridan Dixon, of South Tyneside, was interviewed on ITV Tyne Tees about how she has reduced her drinking as part of efforts to stay cancer free. We’re grateful to our partner Balance North East for helping us share Sheridan’s story.
Wednesday’s highlights

We headed to No 10 Downing St to present our petition to UK Prime Minister Sir Keir Starmer.
Prof Lord John Krebs, Chair of our Global Cancer Update Programme, tabled questions in the Lords on the links between alcohol and cancer, keeping the issue high on the political agenda:
Lord Krebs’ questions to the Lords
-
1
Lord Krebs to ask His Majesty’s Government what steps they are taking to reduce alcohol consumption as a modifiable risk factor for cancer.
-
2
Lord Krebs to ask His Majesty’s Government whether the national cancer plan for England will address alcohol consumption as a modifiable risk factor for cancer.
-
3
Lord Krebs to ask His Majesty’s Government what assessment they have made of public awareness levels of the link between alcohol consumption and cancer risk.
-
4
Lord Krebs to ask His Majesty’s Government what consideration they have given to classifying alcohol as an unhealthy product under high fat, sugar and salt marketing restrictions to (1) strengthen limits on alcohol advertising, and (2) reduce alcohol exposure among vulnerable populations, including children and adolescents.
-
5
Lord Krebs to ask His Majesty’s Government what assessment they have made of the impact of minimum unit pricing on alcohol-related cancer incidence.
CPAW supporter Prof Richard Cooke published research showing that policymakers and drinkers are speaking different languages when it comes to alcohol consumption. He says: “Policymakers need to construct policies to reflect the importance of emotions in drinkers’ narratives. This fits in with psychological theories of drinking behaviour which propose that people drink for different reasons.”
> The language of alcohol: Similarities and differences in how drinkers and policymakers frame alcohol consumption, published in Drug and Alcohol Review
Thursday’s highlights
Health professionals can be instrumental in helping individuals reset their relationship with alcohol and we supported them with a free webinar on Alcohol and cancer risk: What every health professional needs to know.
In the This Is Powerful podcast, Paul Sculfor talked to nutrition expert Dr Federica Amati about alcohol and cancer.
Friday’s highlights
On the blog: It’s mocktail Friday! Start your weekend early with some fizzy fruity creations
Saturday and Sunday’s highlights
Time to take a breath … alcohol is a major part of how many of us socialise, relax and celebrate. But nearly 4% of cancer cases in the UK are down to alcohol – around 17,000 new cases every year.
We hope this Cancer Prevention Action Week has given you an insight into the risks we’re all taking when we drink.
Our research shows that most people don’t know that drinking any amount of alcohol increases the risk of 7 types of cancer.
What happens next?
Cancer Prevention Action Week is just the start. We want to spark an ongoing national debate: with friends, family – and within government – about alcohol and cancer so that everyone can make more informed choices about their health.
But the UK government has said it won’t include mandatory comprehensive restrictions on alcohol marketing in its 10-year Health Plan – despite these being a proven, cost-effective way to reduce alcohol harm.
This is hugely disappointing. Contact the Prime Minister to make it clear that public health must be protected – and that cancer prevention cannot be sidelined.
On the blog
Media coverage
Cancer Prevention Action Week is across the news this week!
-
BBC Radio
Our Senior Policy Advisor, Kendra Chow, was invited to talk about this year’s campaign on BBC 5 Live on Saturday night. The interview was repeated across 5 Live and 43 other BBC radio stations.
-
Channel 5
Vanessa Feltz’s lunchtime show covered alcohol health warnings in a lengthy discussion including an interview with our supporter Dr Philippa Kaye.
Also on Channel 5, Jeremy Vine’s show discussed Alcohol labels should warn of cancer risk, urge health groups (The Times) in a round-up of the morning papers.
-
The Guardian
-
The Independent
-
The Times
-
The Telegraph
-
Julia Bradbury on Instagram
-
Scotland
-
International
- Mirage News (Australia)
- The Times of India
- Yahoo New Zealand
-
Science press
-
Trade press
-
Local press
- Rayo (Coventry and Nuneaton)
- This Is Wiltshire
- The Gazette and Herald
- Swindon Advertiser
- The Birmingham Mail
Facts at your fingertips
Written by experts, based on the evidence: our health resources unmuddle the myths about alcohol and cancer.
The government of the Republic of Ireland must ensure that the planned introduction of alcohol health labels, in May 2026, which are mandated under the Public Health (Alcohol) Act 2018, come into force without delay.
Dr Giota Mitrou, our Executive Director of Research and Policy, has written to Taoiseach Micheál Martin TD and Health Minister Jennifer Carroll MacNeill TD, in support of Ireland’s forthcoming mandatory health warnings labels on alcohol.
We are calling on the Irish government to stand firm on alcohol labelling in the face of misleading representations from the alcohol industry, and resist outside influence. Doing so, Dr Mitrou writes, will solidify Ireland’s record as a world leader on public health and set a much-needed example for other governments across the globe.
Health labels on alcohol crucial to preventing cancer
From 2026, all alcohol products sold in the Republic of Ireland will be required to state: “There is a direct link between alcohol and fatal cancers”. This measure makes Ireland the first country in the world to mandate a warning linking any level of alcohol consumption to cancer.
Yet Ireland is facing resistance to these measures from the alcohol industry in Ireland and worldwide.
Drinking any type of alcohol increases your risk of 7 different types of cancer, and our evidence shows that there is no safe level of drinking.
For Cancer Prevention Action Week 2025, on 23–29 June, we’re highlighting the links between alcohol and cancer and encouraging an open conversation about alcohol’s many harms.
> On the blog: How Ireland beat the odds to introduce cancer warning labels on alcohol
Dr Giota Mitrou
We strongly support alcohol health warning labels. This is not only an evidenced-based policy but also has immense public backing in Ireland, with 70% of those polled supportive of the measure. Crucially, the provision marks a significant step towards the Irish Government fulfilling their duty to protect the public from alcohol harm and reduce preventable cancers.
More on alcohol risks
Alcohol is a proven risk factor for 7 cancer types, and our evidence clearly shows there is no safe level of consumption when it comes to preventing cancer. Each year 17,000 people – 46 people every day – are diagnosed with a cancer caused by alcohol.
Alcohol deaths in England reached nearly 10,500 in 2023, a massive 42% increase since 2019. Despite these tragic statistics, alcohol policy across the UK remains woefully inadequate, doing very little to mitigate its significant harms, including cancer, and the immense burden it places on the NHS.
Making the case for change
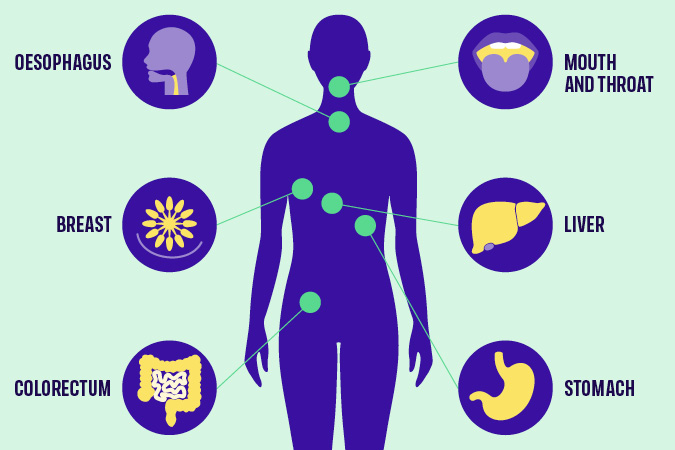
Which cancers are linked to alcohol?
That’s why this year, our flagship campaign – Cancer Prevention Action Week – focuses on the links between alcohol and cancer, aiming to ensure that everyone can make informed decisions about their alcohol consumption. While raising awareness is important, it must be combined with evidenced-based polices that enable and support people to make healthier choices.
As many aspects of alcohol policy are the responsibility of the devolved administrations, Northern Ireland, Scotland and Wales all have alcohol strategies in place. In contrast, England has not had a National Alcohol Strategy since 2012.
We’re calling on the UK government to introduce a long overdue National Alcohol Strategy for England without delay. The Strategy must introduce policies on labelling, pricing and marketing – 3 interventions that have strong evidence of positive impact. Crucially, it must also remain independent of industry influence.
1) Labelling
Despite being carcinogenic, alcohol is exempt from mandatory health warning labels. Unlike other food and drinks, alcohol labels are also not required to include information on nutritional content or calories. As the Alcohol Health Alliance puts it, there is more product information on a bottle of orange juice than on a bottle of beer. In fact, alcoholic drinks only have to display to display minimal information such as the name, strength as alcohol by volume (but only if over 1.2%), allergen information and the best before date (if the drink’s strength is under 10%). Even pregnancy and drink driving warnings are voluntary.
Consumers have a right to know about every product’s health risks and harms. Introducing health warning labels on alcohol that highlight cancer risk, alongside information on nutrition and calories, is an easy and effective way to ensure this. Evidence shows that effective labelling can prompt behaviour change and lead to reduced consumption.
For labelling to be effective, it must be clear, plain, distinct and mandatory. Additionally, labels should not include ambiguous language such as “drink responsibly”. Our policy position on alcohol explains that the use of QR codes to link to health information must be prohibited as, rather than informing people about risks, they provide marketing opportunities by redirecting consumers to producers’ websites.
2) Pricing
Minimum Unit Pricing (MUP) has been introduced in Scotland and Wales, but not in England or Northern Ireland. It sets a baseline price at which a unit of alcohol can be sold and targets cheap, strong alcohol that is often consumed by adolescents and other vulnerable groups.
Public Health Scotland’s review indicates that MUP has reduced alcohol-specific deaths by 13% and averted over 800 hospitals admissions every year since its introduction in 2012. MUP was found to have the most impact on those living in the 40% most deprived areas of Scotland, helping to reduce health inequalities. The Welsh government has also seen the benefits of MUP, which it introduced in 2020. Northern Ireland has consulted on proposals to introduce MUP.
England must follow suit, introducing MUP at 65p and adjusted for inflation thereafter. Without MUP in England, a 2.5 litre bottle of cider containing 19 units of alcohol can be bought for as little at £5.25. Under a 65p minimum unit price, this would rise to £12.19. Industry opposes MUP, arguing that it would damage sales in pubs and restaurants. However, most alcohol sold in these settings is already above minimum unit prices.
3) Marketing restrictions
Marketing restrictions on alcohol remain woefully inadequate. Advertising regulations prohibit linking alcohol with youth, irresponsible behaviour or social success, but enforcement is ineffective. The Advertising Standards Agency has no power to issue fines or sanctions, and often rules on complaints only after a campaign has ended. Like labelling, advertising is not a devolved issue, meaning the picture across the UK is largely the same.
Alcohol advertising is widespread, despite strong evidence linking exposure to alcohol marketing with young people drinking more and at an earlier age. The UK’s insufficient restrictions must be addressed by classifying alcohol as an “unhealthy product” under high fat, sugar or salt (HFSS) marketing restrictions. This would limit its promotion, particularly to vulnerable populations including children and adolescents.
The time to act is now
No family should have to endure the devastating trauma of alcohol-related cancer. Yet, as a result of the rise in high-risk drinking since the coronavirus pandemic, the UK could see more than 18,000 additional cancer cases by 2035.
Join us this Cancer Prevention Action Week to demand action. Sign and share our petition today, calling for a National Alcohol Strategy for England.
- The Alcohol Health Alliance, which we are a member of, has more information on MUP, labelling and marketing restrictions.
Get involved in Cancer Prevention Action Week
Nearly nine in ten Brits (87%) are not aware that drinking red wine increases the risk of cancer, a poll for World Cancer Research Fund has found.
Nearly nine in ten Brits (87%) are not aware that drinking red wine increases the risk of cancer, a poll for World Cancer Research Fund has found.1 The YouGov results have been released for Cancer Prevention Month (1-29 February).
The findings also revealed that nearly three quarters of people (73%) are aware of the link between inherited genes and cancer even though it accounts for less than one in ten cases. Nearly half of people (47%) wrongly thought that stress was directly linked to an increased cancer risk despite evidence discounting this myth.
Our research shows that not drinking alcohol is one of the most important things people can do to reduce their cancer risk, alongside not smoking and being a healthy weight. The latest evidence suggests that the claimed benefits of drinking red wine for heart health are less than previously thought and are outweighed by the harmful effect alcohol has on cancer risk.
The results from the survey showed that many people are still not clear on what increases their risk of cancer. For Cancer Prevention Month, World Cancer Research Fund has an online awareness campaign on whether factors such as cling film, stress and red wine increase cancer risk. This information is to help clarify and give the UK public a better understanding of what factors increase their risk, and what they can do to reduce their risk.

World Cancer Research Fund were the first organisation to identify that diet, weight and physical activity can affect people’s risk of cancer. In fact, a third of the most common cancer cases could be prevented every year in the UK through improved physical activity, diet and weight.
“Cancer is a devastating disease and we are working for a world free of preventable cancers. People are aware of some risk factors, such as inherited genes, but not some of the modifiable lifestyle factors that can really make a difference. With so many people being diagnosed with cancer, we want people to know what factors are increasing their risk, such as red wine, so that they can make informed choices to help reduce their risk.”
Dr Rachel Thompson, Head of Research Interpretation at World Cancer Research Fund
“It is very worrying, but not surprising, that so few people know that red wine increases cancer risk when there are so many contradictory messages out there. All types of alcohol increase the risk of a number of different cancers so we recommend for cancer prevention that people don’t drink any alcohol. In fact, around 21,000 cancer cases could be prevented in the UK every year if no one drank alcohol. We know that it can be hard for people to not drink at all so we’d encourage them to be ‘alcohol savvy’ if they do. For example, add a low-calorie mixer to your alcohol and, in between each alcoholic drink, have a glass of water. It’s also really important to not binge-drink and to spread your weekly limit of seven drinks over a number of days as well as keeping a few days alcohol-free.”
Sarah Toule, Head of Health Information at World Cancer Research Fund
Awareness of the relation between red wine and cancer risk across the UK
When comparing England, Scotland and Wales, the poll showed that Welsh adults are by far the least aware that consuming red wine (5% aware) increases the risk of developing cancer. Regionally, people in the East of England and the North West are the least aware of the link between drinking red and the risk of cancer (both 9%). Out of all age groups 18 to 24 year olds are the most aware (27%) while those most at risk of cancer, the over 55s’, are the least aware (6%).
1 YouGov Plc. Total sample size was 2023 adults. Undertaken between 20 – 23 January 2017. The survey was carried out online. Figures have been weighted and are representative of all GB adults (aged 18+). Available from World Cancer Research Fund