Prof Richard Cooke
Prof Richard Cooke is interested in what motivates people to drink alcohol – he surveys people to find out how psychological variables such as the intention to drink, attitudes about drinking, and regret after drinking alcohol – can predict how much people consume.
“Most of my research has been done with young adults aged 18–30,” says Prof Cooke, “because they were traditionally seen as the group that drinks the most, but this has changed in the last decade. I’m now doing much more research with middle-aged people. I also do studies assessing awareness of drinking guidelines, comparing how young adults and policymakers talk about alcohol, and reviewing the effectiveness of alcohol interventions.”
‘We know it’s dangerous’
“I find alcohol consumption fascinating to study as drinking has high social approval even though we know it’s dangerous. This means that health messages about alcohol are trickier to create than smoking messages. Saying ‘Don’t smoke’ is quite acceptable; saying ‘Don’t drink alcohol’ is less so,” he says.
Prof Cooke has several theories about why alcohol remains so popular across cultures: “Alcohol is a social lubricant: it relaxes people, makes them feel more confident and more able to socialise, especially with strangers. It’s really tied to our psychology in many different, sometimes unexpected, ways.”
A former student of Prof Cooke, Dr Joel Crawford, did his doctorate degree on regret and drinking. He asked young people adults about the fear of missing out (Fomo). When they don’t drink, some people think they are missing out on an enjoyable experience, like missing a party because you have to work. Dr Crawford found that the young adults would rather experience alcohol harms, such as hangovers and feeling sick, than miss events that heavily included alcohol, saying “Fomo was more painful to them than a hangover!”
This study illustrates the social and emotional barriers people trying to drink less may encounter. “It’s the social acceptability of drinking in most situations that makes it a challenge to reduce; drinking is associated with celebrations – birthdays, weddings, getting a new job, becoming a parent– and commiserations – missing out on promotion or the death of a loved one. Alcohol is also linked to healthy activities, like ending a walk in the countryside with a drink in a pub.”
Drinking’s a habit

“At the individual level, drinking habits are an issue. People develop habits when they perform the same behaviour in a stable setting, like drinking every Friday night in the pub with your friends. Breaking this habit means unpicking your routines in ways that people often don’t want to do.”
However, based on current trends, there will be fewer people drinking into middle-age and later life: “This has the potential to dramatically change how we organise events,” says Prof Cooke, comparing it to the rise in the availability and acceptability of non-dairy alternatives to milk. “People will be asking for non-alcoholic drinks at parties, and maybe that will become as acceptable as asking for an alcoholic drink is now.”
Young people prefer to stay in control
We asked Prof Cooke about why there is a decline in young people drinking alcohol. “There are several theories about why this is happening. One is that young people spend a lot of time online, and they want to present the best possible version of themselves as someone who is in control. Studies of Facebook content show that people generally share positive alcohol content, rather than negative experiences.
“Another idea is that alcohol has become more expensive in the last decade or so, which has put young people off drinking. Finally, the rise of energy drinks may be part of the explanation too, especially for young people who like to play games online. Energy drinks, high in caffeine, are likely to aid video game performance. Alcohol is unlikely to do this.”
For people of any age trying to limit their alcohol, Prof Cooke recommends trying to understand the reasons why you drink. “Do you drink to be sociable, to enhance an evening out, to cope with negative emotions? Are there other ways you could meet those needs? Psychological interventions, such as feedback on drinking or setting goals to drink less, can also be effective ways to cut back.”
Prof Cooke’s latest research
Prof Cooke’s latest research is published in Drug and Alcohol Review. He says: “Our new paper shows that policymakers and drinkers talk about drinking in different ways. While policymakers focused on drinking behaviour, drinkers talked about how drinking made them feel different emotions: embarrassed, happy, guilty, sad. Policymakers need to construct policies to reflect the importance of emotions in drinkers’ narratives.”
> Read the paper: The language of alcohol: Similarities and differences in how drinkers and policymakers frame alcohol consumption
Alcohol and cancer: let’s talk
In the UK, alcohol is a major part of how many of us socialise, relax, and celebrate. But do we really know the risks we’re taking when we drink?
Our research shows that most people don’t know that drinking any amount of alcohol increases the risk of 7 types of cancer.
This Cancer Prevention Action Week, we want to spark a national conversation: with friends, family – and within government – about alcohol and cancer.
Cancer Prevention Action Week
This year’s campaign focuses on the links between alcohol and cancer.
You’re socialising with friends. Someone asks what you want. You say: “Oh – I’m not drinking tonight.” And then comes the follow-up:
- Why not?
- Are you on antibiotics?
- Are you pregnant?
- Are you ill?
- Just have one. Come on, it’s Friday.
It’s a scene that plays out thousands of times every weekend in the UK. For a choice that should be straightforward – not having an alcoholic drink – we’ve made it weirdly taboo.
But people say “no thanks” to alcohol for all kinds of reasons.
- They’re trying to sleep better
- They’re dealing with anxiety or illness
- They’re thinking about fertility
- They’ve had a rough week and can’t face a hangover
- They’re training for something
- Or they’re just… not in the mood
And yet that simple choice often triggers awkwardness, suspicion – even ridicule. Why?
Alcohol has become a shortcut for belonging or fear of missing out
So many of us drink to connect, to relax, to mark the end of the day. And saying ‘no’ interrupts that flow. It disrupts the unspoken script: “We’re all doing this together”.
But when choosing not to drink becomes a social problem, we have to ask:
Why is drinking so protected? What are we not talking about?
That’s why – as part of Cancer Prevention Action Week 2025 – we want to get people talking.
‘No thanks’ shouldn’t need a justification
Imagine if we stopped asking people why they’re not drinking – and started asking how can we make not drinking more comfortable for everyone?
Or how can we support them in their choice?
You shouldn’t need to have a serious illness, or be training for a marathon, or whisper that you’re trying for a baby to opt out of alcohol.
And yet, we’ve made not drinking feel like a confession.
This isn’t about demonising alcohol. It’s about giving people the facts and allowing them the space to make different choices – for any reason, or for no reason at all.
Alcohol and cancer: the facts
Alcohol is a Group 1 carcinogen – that means it can cause cancer – putting it in the same category as asbestos, tobacco and plutonium.
Alcohol is directly linked to 7 types of cancer, including:
- Breast
- Bowel
- Liver
- Mouth and throat
- Oesophagus
- Stomach
Even small amounts increase your risk. For example, just 1 drink a day raises your breast cancer risk by around 7–10%. For bowel cancer, the risk starts rising even at low levels of drinking.
But while this science has been clear for years, our polling revealed that 1 in 4 of us don’t associate any health risks with alcohol.
We’re not being given the information we need to make informed choices – and when people do make those choices, they often feel judged, questioned or excluded. That’s wrong.
How do we shift the culture?
1. We normalise ‘No’
We make not drinking visible, valid and unremarkable. The more people hear “No thanks” without a 5-minute explanation, the more normal it becomes.
2. We get curious, not confrontational
When someone doesn’t drink, it’s not a rejection of you – it’s a choice for them. We stop taking it personally. And offer support.
3. We name the stakes
This isn’t just about social awkwardness. It’s about informed choice and health. The cancer link is real, as are the 200 other health conditions associated with alcohol. People deserve to know – and not be made to feel odd when they act on it.
If you’re doing other things to live well – eating healthily, counting your steps, trying to sleep enough – why should people be made to feel awkward about not drinking alcohol?
Ready to change the conversation? Read to say “No thanks”?
Only 16% of us in the UK feel at ease discussing our relationship with alcohol, ranking it among the least talked about topics – less so than sex (17%) and money (29%), according to our poll.
We’re emphasising the connection between alcohol and cancer as part of Cancer Prevention Action Week, which starts today. We have strong evidence that alcohol increases the risk of 7 cancers:
- Breast
- Bowel
- Head and neck
- Oesophageal
- Liver
- Stomach
Alcoholic drinks are also high in calories and often high in sugar, increasing the risk of gaining weight. Living with overweight or obesity increases the risk of at least 13 types of cancer.
We surveyed 2,000 people to gain insights into Britain’s understanding of alcohol and cancer risks. The findings reveal consistent misconceptions regarding alcohol’s dangers. Alarmingly, 25% of respondents did not associate any health risks with alcohol, and only 1 in 14 mentioned cancers as a risk when asked unprompted.
These misconceptions may hinder our ability to have informed conversations about alcohol. About 4% of cancer cases in the UK are attributed to alcohol, meaning that, each year, around 17,000 people are diagnosed with cancer caused by alcohol. Adding to this immeasurable human cost is the economic burden. Alcohol-related cancers cost the NHS around £100m every year.
We need a National Alcohol Strategy
We support clearer public health messaging to raise awareness of the real dangers of alcohol consumption, as well as other measures such as health warning labels. Alongside many other health organisations in the UK, we’re urging the Prime Minister, Sir Keir Starmer, to implement a National Alcohol Strategy for England.
World Cancer Research Fund CEO Rachael Gormley
Alcohol is pervasive in our lives, from celebrations to after-work drinks. But do we truly understand the risks involved? It’s essential that we engage in more discussions about alcohol and cancer, empowering individuals to make informed health choices.
Alcohol Health Alliance Chair Sir Ian Gilmore
One of the reasons public awareness is so low is that we're being kept in the dark about the true cost of drinking. People have the right to know the full picture so that they can make informed choices about what they consume.
World Cancer Research Fund Executive Director of Research and Policy Dr Giota Mitrou
A long-overdue National Alcohol Strategy in England would help the government tackle alcohol harm head on – reducing consumption, lowering cancer risk, and protecting lives.
Nikki Bednall is a World Cancer Research Fund Supporter and breast cancer survivor. She said: “I always thought drinking a few times a week was fine. I never knew it could raise my cancer risk. If I’d known earlier, I might have made different choices. Though hindsight is easy, my perspective has changed with the knowledge that came after my diagnosis.”
Drinking habits in the UK paint a concerning picture in comparison with other nations. Organisation for Economic Cooperation and Development (OECD) 2021 data showed that alcohol consumption in the UK was 10 litres per capita – 16% more than the OECD average of 8.6 litres.
Covid led to an increase in the number of high-risk drinks, with the heaviest drinkers increasing their consumption the most. These changes have persisted beyond the national lockdowns of 2020 and 2021, and subsequently there has been a year-on-year rise in alcohol-specific deaths, which reached an all-time high of 10,473 in 2023.
The research was conducted by Opinion Matters, among a sample of 2,000 nationally representative UK adults. The data was collected between 21.03.2025–24.03.2025.
Cancer Prevention Action Week (CPAW)
This year we’re highlighting the links between alcohol and cancer.
Alcohol and cancer: let’s talk – that was the theme of this year’s Cancer Prevention Action Week. For 7 days on 23–29 June, we talked to politicians, gave radio interviews and spoke to experts about alcohol and cancer. Plus, we shared news and views across our socials:
Facebook | LinkedIn | Instagram | Bluesky
How Cancer Prevention Action Week unfolded
Monday’s highlights
> Brits find it harder to talk about alcohol than sex or money
Yorkshire GP speaks out in support of CPAW:
Dr Nigel Wells, Medical Director and Executive Director Clinical & Care Professional Humber and North Yorkshire ICB and practising GP:
As a GP, I know people can be reluctant to talk about alcohol or share concerns about their drinking – so it doesn’t surprise me that only 2 in 10 people across Yorkshire and the Humber feel comfortable doing so.
But alcohol isn’t harmless – it increases the risk of 7 types of cancer, and, too often, people simply aren’t aware. If this campaign helps someone pause and ask whether alcohol might be affecting their health, and encourages them to speak to a healthcare professional, it will have made a real difference. We need to make these conversations as routine as those about smoking or diet – and that starts with creating a safe, non-judgemental space in every consultation.
We tabled an Early Day Motion in support of Cancer Prevention Action Week. And Alcohol Focus Scotland, a key supporter of this year’s campaign, tabled a motion in the Scottish Parliament on alcohol and cancer.
Tuesday’s highlights

Alcohol Focus Scotland organised a photo call at Holyrood with Members of the Scottish Parliament (MSPs). Photographed are 11 MSPs, including the Cabinet Secretary for Health Neil Gray; Jackie Baillie, Labour’s deputy leader and health spokesperson, and Presiding officer Alison Johnstone. Read more on LinkedIn
Sheridan Dixon, of South Tyneside, was interviewed on ITV Tyne Tees about how she has reduced her drinking as part of efforts to stay cancer free. We’re grateful to our partner Balance North East for helping us share Sheridan’s story.
Wednesday’s highlights

We headed to No 10 Downing St to present our petition to UK Prime Minister Sir Keir Starmer.
Prof Lord John Krebs, Chair of our Global Cancer Update Programme, tabled questions in the Lords on the links between alcohol and cancer, keeping the issue high on the political agenda:
Lord Krebs’ questions to the Lords
-
1
Lord Krebs to ask His Majesty’s Government what steps they are taking to reduce alcohol consumption as a modifiable risk factor for cancer.
-
2
Lord Krebs to ask His Majesty’s Government whether the national cancer plan for England will address alcohol consumption as a modifiable risk factor for cancer.
-
3
Lord Krebs to ask His Majesty’s Government what assessment they have made of public awareness levels of the link between alcohol consumption and cancer risk.
-
4
Lord Krebs to ask His Majesty’s Government what consideration they have given to classifying alcohol as an unhealthy product under high fat, sugar and salt marketing restrictions to (1) strengthen limits on alcohol advertising, and (2) reduce alcohol exposure among vulnerable populations, including children and adolescents.
-
5
Lord Krebs to ask His Majesty’s Government what assessment they have made of the impact of minimum unit pricing on alcohol-related cancer incidence.
CPAW supporter Prof Richard Cooke published research showing that policymakers and drinkers are speaking different languages when it comes to alcohol consumption. He says: “Policymakers need to construct policies to reflect the importance of emotions in drinkers’ narratives. This fits in with psychological theories of drinking behaviour which propose that people drink for different reasons.”
> The language of alcohol: Similarities and differences in how drinkers and policymakers frame alcohol consumption, published in Drug and Alcohol Review
Thursday’s highlights
Health professionals can be instrumental in helping individuals reset their relationship with alcohol and we supported them with a free webinar on Alcohol and cancer risk: What every health professional needs to know.
In the This Is Powerful podcast, Paul Sculfor talked to nutrition expert Dr Federica Amati about alcohol and cancer.
Friday’s highlights
On the blog: It’s mocktail Friday! Start your weekend early with some fizzy fruity creations
Saturday and Sunday’s highlights
Time to take a breath … alcohol is a major part of how many of us socialise, relax and celebrate. But nearly 4% of cancer cases in the UK are down to alcohol – around 17,000 new cases every year.
We hope this Cancer Prevention Action Week has given you an insight into the risks we’re all taking when we drink.
Our research shows that most people don’t know that drinking any amount of alcohol increases the risk of 7 types of cancer.
What happens next?
Cancer Prevention Action Week is just the start. We want to spark an ongoing national debate: with friends, family – and within government – about alcohol and cancer so that everyone can make more informed choices about their health.
But the UK government has said it won’t include mandatory comprehensive restrictions on alcohol marketing in its 10-year Health Plan – despite these being a proven, cost-effective way to reduce alcohol harm.
This is hugely disappointing. Contact the Prime Minister to make it clear that public health must be protected – and that cancer prevention cannot be sidelined.
On the blog
Media coverage
Cancer Prevention Action Week is across the news this week!
-
BBC Radio
Our Senior Policy Advisor, Kendra Chow, was invited to talk about this year’s campaign on BBC 5 Live on Saturday night. The interview was repeated across 5 Live and 43 other BBC radio stations.
-
Channel 5
Vanessa Feltz’s lunchtime show covered alcohol health warnings in a lengthy discussion including an interview with our supporter Dr Philippa Kaye.
Also on Channel 5, Jeremy Vine’s show discussed Alcohol labels should warn of cancer risk, urge health groups (The Times) in a round-up of the morning papers.
-
The Guardian
-
The Independent
-
The Times
-
The Telegraph
-
Julia Bradbury on Instagram
-
Scotland
-
International
- Mirage News (Australia)
- The Times of India
- Yahoo New Zealand
-
Science press
-
Trade press
-
Local press
- Rayo (Coventry and Nuneaton)
- This Is Wiltshire
- The Gazette and Herald
- Swindon Advertiser
- The Birmingham Mail
Facts at your fingertips
Written by experts, based on the evidence: our health resources unmuddle the myths about alcohol and cancer.
The government of the Republic of Ireland must ensure that the planned introduction of alcohol health labels, in May 2026, which are mandated under the Public Health (Alcohol) Act 2018, come into force without delay.
Dr Giota Mitrou, our Executive Director of Research and Policy, has written to Taoiseach Micheál Martin TD and Health Minister Jennifer Carroll MacNeill TD, in support of Ireland’s forthcoming mandatory health warnings labels on alcohol.
We are calling on the Irish government to stand firm on alcohol labelling in the face of misleading representations from the alcohol industry, and resist outside influence. Doing so, Dr Mitrou writes, will solidify Ireland’s record as a world leader on public health and set a much-needed example for other governments across the globe.
Health labels on alcohol crucial to preventing cancer
From 2026, all alcohol products sold in the Republic of Ireland will be required to state: “There is a direct link between alcohol and fatal cancers”. This measure makes Ireland the first country in the world to mandate a warning linking any level of alcohol consumption to cancer.
Yet Ireland is facing resistance to these measures from the alcohol industry in Ireland and worldwide.
Drinking any type of alcohol increases your risk of 7 different types of cancer, and our evidence shows that there is no safe level of drinking.
For Cancer Prevention Action Week 2025, on 23–29 June, we’re highlighting the links between alcohol and cancer and encouraging an open conversation about alcohol’s many harms.
> On the blog: How Ireland beat the odds to introduce cancer warning labels on alcohol
Dr Giota Mitrou
We strongly support alcohol health warning labels. This is not only an evidenced-based policy but also has immense public backing in Ireland, with 70% of those polled supportive of the measure. Crucially, the provision marks a significant step towards the Irish Government fulfilling their duty to protect the public from alcohol harm and reduce preventable cancers.
More on alcohol risks
World Cancer Research Fund has responded to the UK government’s first multi-year spending review, where the Chancellor, Rachel Reeves, set out departmental budgets over the next 3 years.
Under their Health Mission, the government has committed to shifting from sickness to prevention, affirming that prevention is better than cure. This spending review marks a critical opportunity for the government to set out their investment to this commitment.
In this review, the Chancellor committed:
- £29bn for the day-to-day spending of the NHS to 2028–29.
- £80m per year for tobacco cessation programmes and to support the delivery of the Tobacco & Vapes Bill.
- £10bn in NHS technology and digital transformation by 2028–29.
- £22.6bn per year for research and development by 2029–30, including medical research.
Responding to the spending review, World Cancer Research Fund’s Executive Director of Research and Policy, Dr Giota Mitrou, said:
Today the Chancellor reaffirmed Labour’s Health Mission, including their commitment to shift from treatment to prevention. 40% of all cancer cases are preventable: as leading experts in cancer prevention, we know that primary prevention remains the most sustainable and cost-effective way to tackle cancer and other non-communicable diseases.
For example, while we are glad to see that the government will be investing £80m per year to tackle tobacco, we need to see similar efforts applied to obesity and alcohol. The expansion of free school meals is a step in the right direction and the type of action we hope to see in the upcoming 10-year Health Plan.”
Research funded by World Cancer Research Fund has shown that people living with cancer who closely follow a sustainable and nutritious diet – the EAT-Lancet reference diet – have a lower risk of dying from cancer and from all causes.
This is the first study to look at the impact of the EAT-Lancet diet on people living with or beyond cancer – as opposed to the general population. Prof Sabine Rohrmann and her team at the University of Zurich, in collaboration with colleagues from another Swiss university, the UK and Austria, used UK Biobank data to see if closely following this diet – with its emphasis on eating a rich variety of plant foods – affected the risk of death for people with a cancer diagnosis at the time they were recruited for the study.
Studying more than 25,000 people with an average age of 60 years at recruitment, the researchers used dietary information collected in the UK Biobank to develop a score that reflected how closely participants followed the EAT-Lancet diet.
More support needed for people facing cancer
Of the 25,348 cancer survivors in the group studied, 4,781 people died during the study follow-up. Prof Rohrmann’s results showed modest links between closely following the diet and a lower risk of dying from cancer, and of dying from all causes. The researchers didn’t observe a link between the diet and dying from heart disease.
Almost 64% of the participants were female, and participants who followed the EAT-Lancet diet more closely were more likely to be female. However, this study confirmed previous evidence showing that people living with and beyond cancer do not tend to follow healthy diets after their diagnosis. This emphasises the need to help people form healthier habits and overcome the barriers to eating well, such as treatment side-effects affecting appetite and taste.
These findings highlight the importance of greater nutrition support and guidance for people facing cancer. Guidelines aimed at the general population are unlikely to consider the needs of people living with and beyond cancer. With a lack of evidence-based recommendations for this population, the gap can sometimes be filled by practices not supported by the science – such as excessive use of dietary supplements.
This evidence showing the benefits of the EAT-Lancet diet follows recent research by our Global Cancer Update Programme, which provided guidance for people with a breast or a bowel cancer diagnosis.
Prof Sabine Rohrmann
We specifically put the focus of our study on cancer survivors because we believe that it is important to encourage them to follow a healthy lifestyle. For this, we need more evidence and so far, research on lifestyle changes in cancer survivors is still scarce.
Dr Julia Panina, Head of Research Funding
This study provides important new evidence that following the EAT-Lancet reference diet may reduce the risk of mortality in people living with and beyond cancer. The focus on the consumption of plant-based foods reflects our Cancer Prevention Recommendations to eat more wholegrains, vegetables, fruit and beans, and to limit red and processed meat. Importantly, these findings also show that diets supporting cancer survivorship can promote more sustainable eating and help protect the environment.
The EAT-Lancet reference diet was created by a team of scientists (The EAT-Lancet Commission on Food, Planet, Health) in 2019. It is a mainly plant-based diet that, according to the Commission, addresses the environmental impact of food production and consumption better than most national dietary guidelines.
> Read the paper: Higher adherence to the EAT-Lancet reference diet is inversely associated with mortality in a UK population of cancer survivors
> On the blog: Plant-based diets: eating for our health and the planet
Researchers funded by World Cancer Research Fund have discovered that brisk walking is linked to a lower risk of 5 cancers:
- anal
- liver (hepatocellular carcinoma)
- small intestine
- thyroid
- lung
Using information stored in the UK Biobank – a large database of many different aspects of health – scientists explored the link between walking pace – slow, steady or brisk – and the risk of developing 28 types of cancer.
They confirmed that the link between brisk walking and a reduced risk of developing the 5 cancers was true, even after accounting for overall physical activity and total walking time.
Speeding up your walk could represent an easy, low-cost public health intervention to decrease cancer risk.
The paper, published in BMC Cancer, says:
“Adopting a brisk walking pace may represent a pragmatic target for public health interventions to decrease cancer risk, particularly in circumstances where increases in walking volume or frequency prove impractical.”
PhD student Michael Stein’s research was supported by funding from Prof Michael Leitzmann’s grant. This research was funded by World Cancer Research Fund as part of the WCRF International Regular Grant Programme.
> Read the full paper: Usual walking Pace and risk of 28 cancers– results from the UK biobank
 John Steventon is our very own supporter superhero. He completed a HYROX in December dressed as comic book character Wolverine, alongside a friend who dressed as Deadpool – and he isn’t stopping there.
John Steventon is our very own supporter superhero. He completed a HYROX in December dressed as comic book character Wolverine, alongside a friend who dressed as Deadpool – and he isn’t stopping there.
HYROX is an indoor fitness race enhanced by workout stations along the route, so competitors run 1km, then do a workout – 8 times! The workouts include rowing, pulling and pushing a sled, and lunges while carrying a sandbag, making it an exhausting but fun challenge.
John said: “Everything I’ve done in life, I’ve wanted to share with others. As a DJ, I taught aspiring musicians and even wrote DJing for Dummies. In my TV career, I mentor new editors. When I was racing in indoor rowing, I launched the RowAlong YouTube channel to help home rowers stay motivated. So, when I started competing in HYROX, I wondered how I could use this platform to make a difference. “
“I knew I’d never be a podium finisher, but after my skin cancer diagnosis, I found a purpose: racing as Wolverine to raise money for World Cancer Research Fund. The response from the HYROX community has been incredible – not just in donations, but in the conversations I’ve had. Nearly everyone I meet has been touched by cancer in some way, whether personally or through friends and family.”
‘I thought I was invincible’
“Even though the doctor said, “Don’t worry”, when I heard the words “That’s skin cancer” the last hope that I was indestructible fizzled away. I’d always thought I was invincible – after all, I like to dress up as Wolverine – but skin cancer reminded me that none of us are.”
John’s diagnosis helped him become more aware of the importance of cancer prevention. “I remember being 7 years old, resisting my Mum’s attempts to put sun cream on me. I often opted for the lowest SPF possible, thinking sunburn was just a fast track to a tan. Coming from Scotland, where sunshine is a rarity, I’ve always craved the sun’s warmth. But now, I never go without factor 30 or 50. If only I had learned that lesson earlier.
“The guidance from the World Cancer Research Fund has been invaluable in helping me understand the importance of proper nutrition and lifestyle choices in cancer prevention and overall health. Exercise alone isn’t enough – we need to fuel ourselves properly and protect ourselves from preventable risks like excessive sun exposure.”
John continues to take on HYROX challenges to raise money for us. He’s completed 3, including one in Frankfurt, and is running The Grid competition again in September, as well as more HYROX events this year. So far, he’s raised nearly £2,000 towards cancer prevention – thank you, John!
Having a greater weight at birth, or a higher body size as a child, adolescent or young adult, is associated with an increased risk of bowel cancer (also known as colorectal cancer) in later life, according to new analysis by World Cancer Research Fund International.
In a major review, looking at 37 studies, our experts discovered that a higher body mass index (BMI) in childhood (2–9 years), adolescence (10–19 years), and young adulthood (18–25 years) increased bowel cancer risk during adulthood. A higher birthweight was also associated with a higher bowel cancer risk.
Innovative research
This work is part of our Global Cancer Update Programme (CUP Global). The paper is published today in the International Journal of Cancer.
The review was conducted by researchers at Wageningen University & Research (WUR) in the Netherlands. It is the first review to analyse and judge all the research examining how factors such as weight, height and body size in early life relate to our risk of bowel cancer as we get older. The results of the study were judged by our CUP Global Expert Panel.
> More information about how we judge the evidence and our evidence grading criteria.
Dr Helen Croker, Assistant Director of Research and Policy
Cancer is a complex disease which develops over several decades, so better understanding of its early origins is critical for more effective prevention and understanding the research gaps. This study shows that a higher body mass index across childhood through young adulthood is an important risk factor for colorectal cancer.
Dr Dieuwertje Kok, Associate Prof of Nutrition and Cancer at WUR
The team was excited to review results from 37 publications that explored birthweight, as well as body mass index across different early life stages. This study bridges the existing knowledge gap and enhances our understanding of how early life factors may affect colorectal cancer risk in adults.
CUP Global is the world’s largest and most authoritative source of research on cancer prevention and living with and beyond cancer. It’s a rigorous, systematic programme that gathers, analyses and assesses global research on how diet, nutrition, physical activity and body weight affect cancer risk and survival.
CUP Global is funded by the World Cancer Research Fund network of charities: American Institute for Cancer Research, World Cancer Research Fund and Wereld Kanker Onderzoek Fonds (WKOF). The review informing this work was funded by WKOF through a CUP Global collaboration with WUR.
Our research portfolio spans a wide range of areas within cancer prevention. Today we’re spotlighting a lab-based study taking place in Newcastle. Local MP Chi Onwurah met Assoc Professor Jill McKay, Prof Dianne Ford and Dr Jessica Saville from Northumbria University, to discuss their groundbreaking cancer prevention research.
Hosted at the university, Chi learned about cancer prevention at the molecular level through her engagement with Assoc Prof Jill McKay and her team. World Cancer Research Fund awarded the team a £347,000 grant to conduct a laboratory-based study investigating whether folate levels in expectant mothers are linked to the development of leukaemia in their children. Folate is a B-vitamin naturally found in green leafy vegetables and liver, while its synthetic form, folic acid, is commonly used in supplements and fortified foods. Some studies suggest folic acid supplementation during pregnancy may help prevent childhood leukaemia; however, findings are not yet clear.
Leukaemia, a cancer of the blood, is the most common childhood cancer worldwide, responsible for 1 in 3 childhood cancers, and rates are slowly increasing. This important research could identify biological markers to help screen or monitor children at increased risk. Ultimately this could lead to earlier diagnosis, which is closely tied to better outcomes for leukaemia patients. It could also result in improved nutritional guidelines for pregnancy.
Assoc Prof Jill McKay, Principal investigator, Northumbria University
Rates of childhood leukaemia are slowly rising, which suggests some things in our environment may be contributing to this disease developing. Learning more about what factors can affect leukaemia and how they influence underlying biology can help us know which lifestyle changes we can make to aim to prevent and predict childhood leukaemia. However, none of this will be possible unless we liaise with policy makers, so we are delighted to meet with Chi today to share our exciting research.
Importantly, the researchers and MP discussed the study’s potential to influence nutritional guidelines during pregnancy, reduce the risk of childhood leukaemia, and support earlier diagnosis. As Chair of the Science, Innovation and Technology Committee, Chi Onwurah MP was particularly interested in hearing about the study’s progress, upcoming publications, and future plans following its completion.
Dr Jana Sremanakova, Research Funding Manager, WCRF International
This is a particularly exciting and important moment for us at the World Cancer Research Fund, as it marks the first time we are connecting our grant holders directly with their MP. It’s a unique opportunity to highlight the impact of our work in cancer prevention research and our national cancer prevention efforts.
Alcohol is a proven risk factor for 7 cancer types, and our evidence clearly shows there is no safe level of consumption when it comes to preventing cancer. Each year 17,000 people – 46 people every day – are diagnosed with a cancer caused by alcohol.
Alcohol deaths in England reached nearly 10,500 in 2023, a massive 42% increase since 2019. Despite these tragic statistics, alcohol policy across the UK remains woefully inadequate, doing very little to mitigate its significant harms, including cancer, and the immense burden it places on the NHS.
Making the case for change
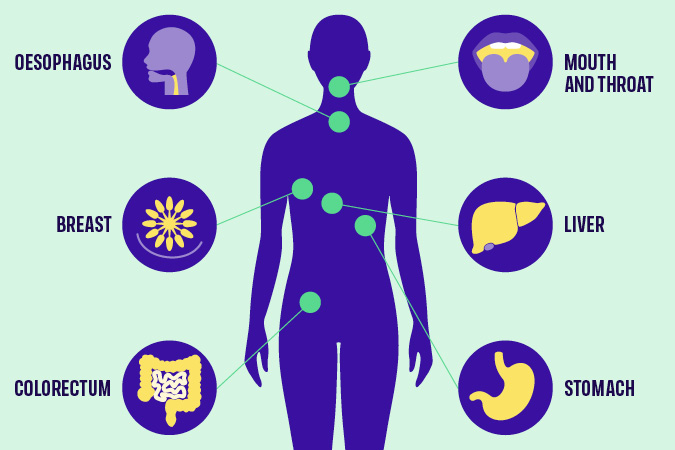
Which cancers are linked to alcohol?
That’s why this year, our flagship campaign – Cancer Prevention Action Week – focuses on the links between alcohol and cancer, aiming to ensure that everyone can make informed decisions about their alcohol consumption. While raising awareness is important, it must be combined with evidenced-based polices that enable and support people to make healthier choices.
As many aspects of alcohol policy are the responsibility of the devolved administrations, Northern Ireland, Scotland and Wales all have alcohol strategies in place. In contrast, England has not had a National Alcohol Strategy since 2012.
We’re calling on the UK government to introduce a long overdue National Alcohol Strategy for England without delay. The Strategy must introduce policies on labelling, pricing and marketing – 3 interventions that have strong evidence of positive impact. Crucially, it must also remain independent of industry influence.
1) Labelling
Despite being carcinogenic, alcohol is exempt from mandatory health warning labels. Unlike other food and drinks, alcohol labels are also not required to include information on nutritional content or calories. As the Alcohol Health Alliance puts it, there is more product information on a bottle of orange juice than on a bottle of beer. In fact, alcoholic drinks only have to display to display minimal information such as the name, strength as alcohol by volume (but only if over 1.2%), allergen information and the best before date (if the drink’s strength is under 10%). Even pregnancy and drink driving warnings are voluntary.
Consumers have a right to know about every product’s health risks and harms. Introducing health warning labels on alcohol that highlight cancer risk, alongside information on nutrition and calories, is an easy and effective way to ensure this. Evidence shows that effective labelling can prompt behaviour change and lead to reduced consumption.
For labelling to be effective, it must be clear, plain, distinct and mandatory. Additionally, labels should not include ambiguous language such as “drink responsibly”. Our policy position on alcohol explains that the use of QR codes to link to health information must be prohibited as, rather than informing people about risks, they provide marketing opportunities by redirecting consumers to producers’ websites.
2) Pricing
Minimum Unit Pricing (MUP) has been introduced in Scotland and Wales, but not in England or Northern Ireland. It sets a baseline price at which a unit of alcohol can be sold and targets cheap, strong alcohol that is often consumed by adolescents and other vulnerable groups.
Public Health Scotland’s review indicates that MUP has reduced alcohol-specific deaths by 13% and averted over 800 hospitals admissions every year since its introduction in 2012. MUP was found to have the most impact on those living in the 40% most deprived areas of Scotland, helping to reduce health inequalities. The Welsh government has also seen the benefits of MUP, which it introduced in 2020. Northern Ireland has consulted on proposals to introduce MUP.
England must follow suit, introducing MUP at 65p and adjusted for inflation thereafter. Without MUP in England, a 2.5 litre bottle of cider containing 19 units of alcohol can be bought for as little at £5.25. Under a 65p minimum unit price, this would rise to £12.19. Industry opposes MUP, arguing that it would damage sales in pubs and restaurants. However, most alcohol sold in these settings is already above minimum unit prices.
3) Marketing restrictions
Marketing restrictions on alcohol remain woefully inadequate. Advertising regulations prohibit linking alcohol with youth, irresponsible behaviour or social success, but enforcement is ineffective. The Advertising Standards Agency has no power to issue fines or sanctions, and often rules on complaints only after a campaign has ended. Like labelling, advertising is not a devolved issue, meaning the picture across the UK is largely the same.
Alcohol advertising is widespread, despite strong evidence linking exposure to alcohol marketing with young people drinking more and at an earlier age. The UK’s insufficient restrictions must be addressed by classifying alcohol as an “unhealthy product” under high fat, sugar or salt (HFSS) marketing restrictions. This would limit its promotion, particularly to vulnerable populations including children and adolescents.
The time to act is now
No family should have to endure the devastating trauma of alcohol-related cancer. Yet, as a result of the rise in high-risk drinking since the coronavirus pandemic, the UK could see more than 18,000 additional cancer cases by 2035.
Join us this Cancer Prevention Action Week to demand action. Sign and share our petition today, calling for a National Alcohol Strategy for England.
- The Alcohol Health Alliance, which we are a member of, has more information on MUP, labelling and marketing restrictions.